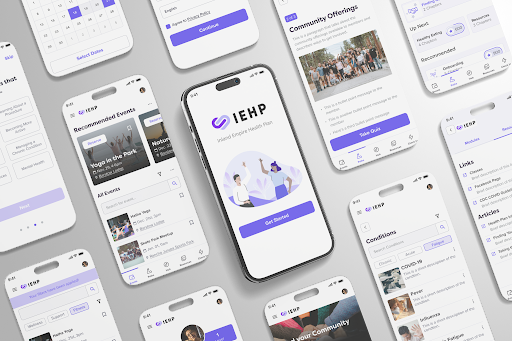

Healthcare Platform
Inland Empire Health Plan (IEHP) is a not-for-profit Medi-Cal and Medicare health plan that provides comprehensive health care coverage to more than 1.2 million Inland Empire residents. Armed with a network of more than 6,000 providers and 2,000 team members, IEHP is the largest health plan in the Inland Empire and one of the fastest-growing health plans in the United States.
The Challenge
Inland Empire Health Plan serves more than 1.2 million Medi-Cal and Medicare members across Southern California. As a not-for-profit health plan with over 6,000 providers in its network, IEHP was facing a reality that most health plans confront: 80% of health outcomes are driven by what happens outside the doctor's office.
The data painted a clear picture. Members with unmet social needs had 60% greater prevalence of diabetes. Half of Americans struggle to find affordable, healthy food. And 36% of adults in the US have low health literacy, creating barriers to managing their own care.
IEHP wanted to offer services comparable to high-end commercial health plans, but their members faced challenges those plans rarely addressed. Many spoke Spanish as their primary language. Most used Android devices. And the traditional model of care wasn't touching the social determinants that were driving poor health outcomes and downstream costs.
The health plan needed a way to meet members where they were, connect them to community resources, and make health management accessible for people with varying levels of health literacy.

Our Approach
We started with a fundamental question: how do you influence the 80% of health that happens outside clinical settings?
The solution couldn't just be another patient portal. IEHP's members needed something that addressed food insecurity, connected them to community workshops, made health education engaging rather than overwhelming, and did all of this in both English and Spanish.
We designed with IEHP's specific user base in mind. That meant Android-first development to match their members' device usage. It meant bilingual functionality from day one, not as an afterthought. And it meant keeping the interface simple and accessible, with minimal flashy styling that might confuse users with lower digital literacy.
The platform needed to pull real health data from EHRs while also connecting members to Community Based Organizations. It needed to make learning about diabetes management as engaging as a mobile game. And it needed to give IEHP visibility into member needs so care teams could intervene proactively.

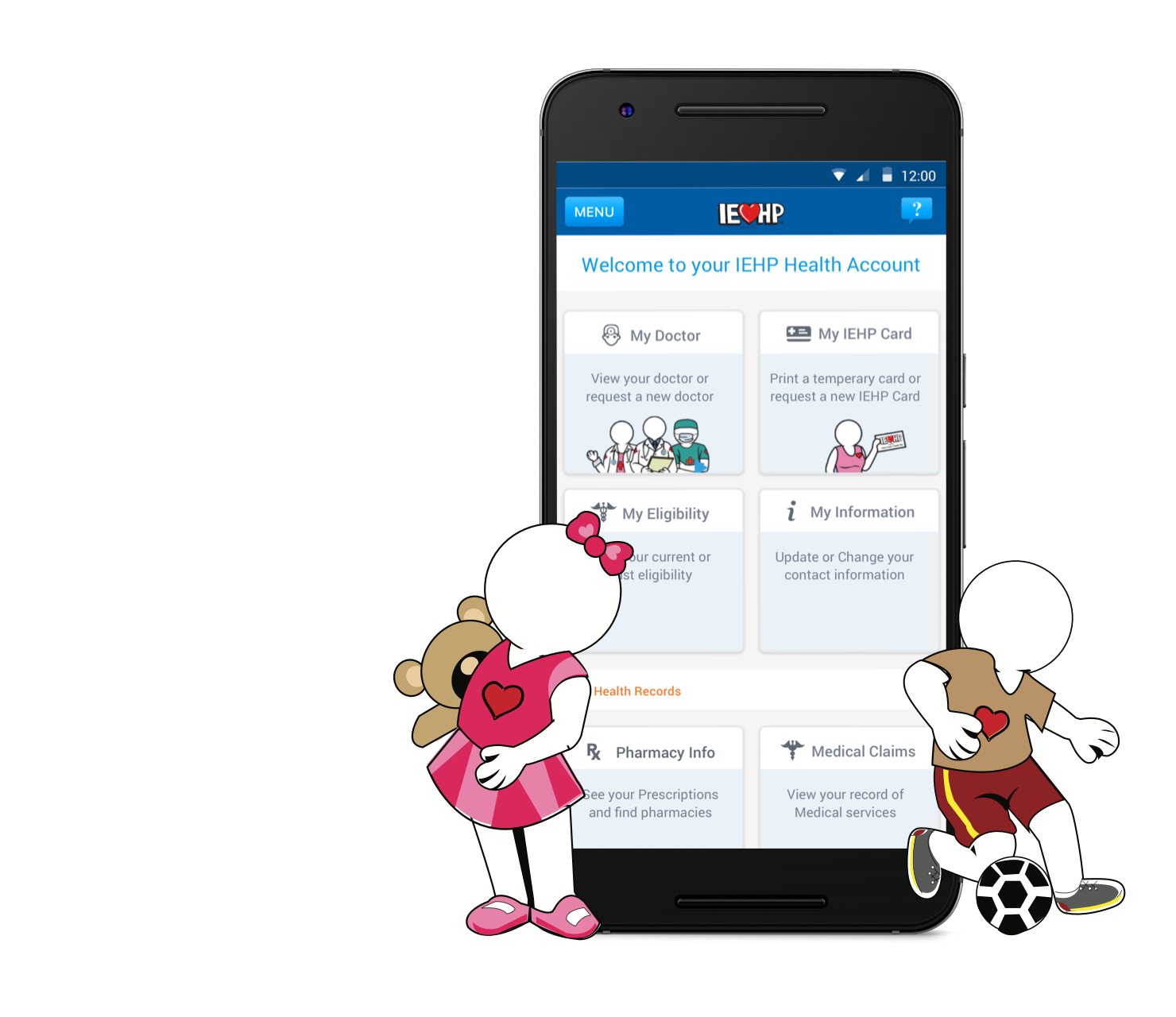
View Health Records

Find a Doctor

Manage Claims
What We Built
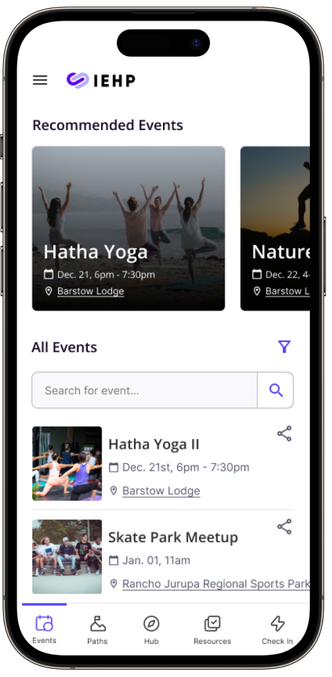
 Health Hub and Events. Health Hub gives members a multilingual view of EHR-pulled clinical data, wearable metrics so they can focus on what matters. Events let members discover, register, save to calendar and get reminders for local workshops and classes.
Health Hub and Events. Health Hub gives members a multilingual view of EHR-pulled clinical data, wearable metrics so they can focus on what matters. Events let members discover, register, save to calendar and get reminders for local workshops and classes.
 Education and Resources. Modular, adaptive learning surfaces condition-specific education to build health literacy and motivate preventive action. Integrated resource directories connect members to vetted community organizations for food, housing and social needs.
Education and Resources. Modular, adaptive learning surfaces condition-specific education to build health literacy and motivate preventive action. Integrated resource directories connect members to vetted community organizations for food, housing and social needs.
 Gamification and Integrated Care. Behavioral-science gamification, badges and real-world incentives drives sustained engagement and turns learning into action.
Gamification and Integrated Care. Behavioral-science gamification, badges and real-world incentives drives sustained engagement and turns learning into action.
Outcomes
The platform achieved over 90,000 installs across both the member app and IEHP's Community Hub, demonstrating strong adoption in a population that historically faces barriers to digital health tools.
More importantly, IEHP now has a direct channel to influence the 80% of health that happens outside clinical settings. Members who previously struggled to navigate the healthcare system can now access community resources, manage their care plans, and build health literacy at their own pace. The bilingual interface removed language as a barrier to health information, addressing a critical equity gap.
The gamification and education modules transformed how members engage with preventive care. Rather than waiting for health issues to escalate, members now have tools and incentives to take proactive steps. And IEHP's care teams gained visibility into member behaviors and social needs, enabling earlier, more targeted interventions that reduce downstream healthcare costs.