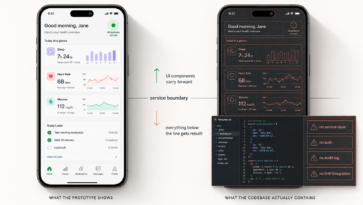
Most healthcare organizations evaluate app developers the same way they’d evaluate any software vendor: portfolio, price, timeline. But healthcare app development isn’t generic software development, and the firms worth hiring aren’t dev shops, they’re strategic product partners who help you figure out what to build before they build it. These 15 questions separate the two.
Clutch Rating
(48+ Reviews)
Healthcare Implementations
(14 Years)
Client PortCo
Value Created
Last updated: May 2026
By: Josh Koenig, Product & Strategy, Sidebench
Questions 1-5: Architecture and HIPAA Compliance
The first five questions test whether a developer treats HIPAA as an architecture decision or a hosting checkbox. Healthcare data breaches cost $9.77 million per incident on average (IBM 2024), and the vast majority of failures happen at the application layer, not the infrastructure layer.
1. “Where in your application stack does PHI reside, and how do you protect it at each layer?”
This question tells you immediately whether the developer understands application-layer security. A good answer walks through data at rest, in transit, and in processing, and names specific controls at each layer (AES-256 encryption, TLS 1.3 for transit, field-level encryption for high-sensitivity data). A bad answer mentions AWS HIPAA compliance or “we use a BAA” without getting more specific.
Red flag: “Our cloud provider handles HIPAA compliance.”
2. “How do you implement access controls for applications that serve multiple user roles?”
Healthcare apps typically serve 4-6 user types (patients, clinicians, administrators, billing staff, family members, supervisors). Each needs different data views and different permissions. The developer should describe role-based access control (RBAC) or attribute-based access control (ABAC) and explain how they handle permission inheritance, session management, and the principle of least privilege.
Red flag: “We’ll figure out permissions during testing.”
3. “What does your audit logging implementation look like?”
HIPAA’s Security Rule (45 CFR 164.312(b)) requires audit controls that record and examine access to PHI. Ask specifically: what events get logged? How long are logs retained? Can you produce a complete access history for a specific patient record? Tamper-proof logging isn’t optional. If the developer hasn’t built it before, they’ll underestimate the effort.
Red flag: “We log errors and exceptions” (that’s debugging, not HIPAA audit logging).
4. “How do you handle the BAA chain from subcontractors through to deployment?”
HIPAA requires Business Associate Agreements not just between you and the developer, but between the developer and every subcontractor who touches PHI. That includes hosting providers, third-party APIs, analytics tools, and monitoring services. A developer who hasn’t navigated this before will miss links in the chain, and you’ll carry the liability.
Red flag: “We sign a BAA with you. That covers everything.”
5. “Walk me through your breach notification process.”
Under the HIPAA Breach Notification Rule, covered entities must report breaches within 60 days. Your development partner needs a documented process: detection, containment, forensic analysis, notification, and remediation. This isn’t hypothetical, it’s a question of when, not if. The developer should have a specific incident response plan, not a vague commitment to “notify you immediately.”
Red flag: Long pause followed by generic reassurance.
Questions 6-10: Healthcare Domain Experience
Healthcare isn’t a vertical you can fake. The regulatory complexity (HIPAA, 42 CFR Part 2, FDA SaMD), the clinical workflow requirements, and the multi-stakeholder dynamics require experience that can’t be replaced by technical talent alone.
6. “Which healthcare EHR systems have you integrated with, and what were the timelines?”
EHR integration is where most healthcare projects stall. A developer with real experience will name specific systems (Epic, Cerner/Oracle Health, CentralReach, athenahealth), describe the integration approach (FHIR, HL7v2, proprietary APIs), and give realistic timelines (3-6 months for a major EHR connection). Vague answers about “API integration” suggest they haven’t done it in healthcare.
Red flag: “We can integrate with any system through APIs” with no healthcare-specific examples.
7. “Can you share specific outcome metrics from your healthcare projects?”
Not “we built an app” but “we reduced patient waitlists by 83%” or “we improved intake completion rates by 40%.” Outcome metrics prove the developer understands healthcare value creation, not just software delivery. If they can only share technical deliverables and timelines without business or clinical outcomes, they’re building features, not solving problems.
Red flag: “We delivered on time and on budget” with no outcome data.
8. “How do you approach clinical workflow design?”
Healthcare applications succeed or fail based on whether they fit into existing clinical workflows. The developer should describe a discovery process that involves shadowing clinical staff, mapping existing workflows, and identifying friction points before writing code. “User research” isn’t enough, you need clinical workflow research conducted by people who understand care delivery.
Red flag: “We’ll gather requirements from your project manager.”
9. “What regulatory frameworks beyond HIPAA have you worked within?”
Depending on your product, you might need compliance with 42 CFR Part 2 (substance use disorder data), FDA SaMD guidelines (if making clinical claims), state telehealth licensing requirements, or payer-specific reporting standards. A developer who only knows HIPAA will miss requirements that surface mid-project, and missed requirements become expensive change orders.
Red flag: Blank stare when you mention 42 CFR Part 2 or SaMD.
10. “What’s the most complex healthcare scheduling problem you’ve solved?”
Scheduling reveals healthcare operational maturity fast. Simple booking is easy. Multi-provider coordination with insurance authorization tracking, supervision ratio compliance, and cross-site resource allocation, that’s a different problem. If your project involves scheduling (and most healthcare apps touch scheduling eventually), the developer needs to demonstrate they understand the constraint-satisfaction nature of healthcare scheduling.
Red flag: “We used Calendly/Cal.com with some customization.”
Questions 11-15: Delivery Model and Outcome Evidence
The best HIPAA architecture and deepest healthcare experience mean nothing if the delivery model doesn’t fit your organization. These five questions test team structure, communication approach, and how the developer handles the messy reality of healthcare product delivery.
11. “Who exactly will work on my project, and what’s their healthcare experience?”
Ask for names. Ask for bios. Agencies often pitch with their A-team and deliver with juniors. In healthcare, that’s dangerous, a developer without HIPAA training or clinical workflow understanding will make mistakes that cost months to fix. You want senior architects with healthcare experience on the project, not just in the company.
Red flag: “We’ll assign the right team once the contract is signed.”
12. “How do you handle scope changes when clinical requirements evolve mid-project?”
Clinical requirements always evolve. Regulatory guidance changes. Payer requirements shift. Clinical staff discover workflow issues during testing. A good developer expects this and has a change management process that evaluates impact, adjusts timelines, and communicates trade-offs clearly. A bad one treats every change as a billable scope expansion.
Red flag: “Changes go through formal change orders with additional billing.”
13. “What does your post-launch support model look like?”
Healthcare apps don’t ship and stop. They need ongoing compliance monitoring, security patching, EHR API version updates, and feature evolution as clinical requirements change. Ask specifically: what SLAs do you offer? How do you handle emergency security patches? What’s the cost structure for ongoing maintenance vs. new feature development?
Red flag: “We offer a 30-day warranty period.”
14. “How do you measure project success?”
A healthcare-focused developer measures success in clinical and business outcomes: patient engagement rates, clinical outcome improvements, operational efficiency gains, payer contract readiness. A generic developer measures success in delivered features and sprint velocity. Same work, completely different definition of “done.”
Red flag: “Success is delivering the agreed scope on time.”
15. “Can I speak with a reference at a healthcare organization you’ve worked with?”
This is non-negotiable. Not a testimonial on their website. An actual conversation with a CTO, CIO, or VP of Engineering at a healthcare organization they’ve worked with. Ask the reference: would you hire them again? What went wrong? How did they handle it? References filter out the majority of vendors who look good on paper but don’t perform in healthcare’s complex reality.
Red flag: “We can share some case studies instead.”
Red Flag Summary: Good Answers vs. Bad Answers
| Question Area | Good Answer Sounds Like | Red Flag Sounds Like |
|---|---|---|
| PHI protection | “We use field-level encryption with AES-256, TLS 1.3, and key rotation…” | “Our cloud provider handles that” |
| Access controls | “We implement RBAC with role inheritance and scope-based data filtering…” | “We’ll add permissions in testing” |
| EHR integration | “We’ve integrated with Epic via FHIR R4 and CentralReach. Timeline was 4 months…” | “We can integrate with any API” |
| Outcomes | “We reduced waitlists by 83% and improved conversion by 40%…” | “We delivered on time and on budget” |
| Clinical workflows | “We shadow clinical staff during discovery and map every handoff…” | “Send us the requirements doc” |
| Team structure | “Here’s who’ll be on your project: [names and bios]…” | “We’ll assign the right team later” |
| Post-launch | “We offer ongoing SLAs with 4-hour response for critical security issues…” | “30-day warranty included” |
| References | “Here are three healthcare CTOs you can call this week…” | “Check our case studies” |
Key Takeaways
- HIPAA is an architecture decision, not a hosting decision. Questions 1-5 test whether the developer understands application-layer compliance.
- Healthcare experience can’t be faked. Questions 6-10 test EHR integration history, clinical workflow design, and regulatory depth.
- Delivery model matters as much as technical skill. Questions 11-15 test team structure, change management, and how success is measured.
- Demand outcome metrics, not just deliverables. “Reduced waitlists by 83%” beats “delivered 47 user stories” every time.
- Always talk to references. Not testimonials. Real conversations with healthcare CTOs and CIOs.
FAQ
How many healthcare app developers should I evaluate?
3-5 is the sweet spot. Fewer than three doesn’t give you enough comparison points. More than five burns evaluation time without improving the decision. Use these 15 questions as a structured scorecard across all candidates to make the comparison objective.
Should I prioritize healthcare experience over technical skill?
Yes, with a caveat. Healthcare experience without strong technical execution delivers compliant but poorly-built products. But technical excellence without healthcare knowledge is more dangerous, they’ll build the wrong thing efficiently. Look for teams that combine both. The healthcare context shapes what you build. The technical skill determines how well you build it.
How do I verify a developer’s HIPAA compliance claims?
Ask for specifics. Request their security control documentation. Ask which third-party security assessments they’ve completed (SOC 2 Type II, HITRUST are common). Ask for their incident response plan in writing. And critically, ask for a reference at a healthcare organization where they’ve passed a security audit or payer compliance review. Claims are easy. Evidence is harder to fake.
What’s a reasonable budget for a HIPAA-compliant healthcare app?
$250K-$750K for an MVP with HIPAA architecture, one or two EHR integrations, multi-role access, and outcomes tracking. Simpler projects (patient portal, single-purpose app) can land in the $150K-$300K range. Complex platforms with multiple EHR integrations, scheduling, and multi-site support run $500K-$1M+. Developers quoting significantly below these ranges are likely missing compliance requirements that’ll surface as change orders later.
How long should healthcare app development take?
4-8 months for an MVP, depending on complexity. That includes discovery, design, and technical architecture (6-10 weeks), and engineering (12-24+ weeks). EHR integrations can add 3-6 months. If a developer promises a HIPAA-compliant healthcare app in 8 weeks, be skeptical, they’re probably skipping compliance architecture that you’ll need before your first payer contract.
Should I choose a healthcare-specialized developer or a generalist?
Healthcare-specialized for anything that touches PHI, requires EHR integration, or needs payer compliance. The regulatory overhead and clinical workflow complexity create a learning curve that generalists underestimate. Generalists are fine for patient-facing marketing sites, content platforms, or internal tools that don’t handle clinical data.
What’s the biggest risk when hiring a healthcare app developer?
Selecting a vendor based on price and portfolio without testing compliance depth and healthcare experience. The most common failure mode: a developer delivers a functional app that can’t pass a payer security review, doesn’t integrate with the health system’s EHR, or doesn’t meet HIPAA requirements at the application layer. Fixing these gaps post-build costs 2-3x more than building them correctly from the start.
How do I evaluate offshore vs. US-based healthcare development teams?
Purely offshore teams can be excellent for general software development, but healthcare adds complications: HIPAA requires specific training and access controls for anyone who touches PHI, time zone differences complicate clinical workflow discovery sessions, and regulatory nuance is harder to communicate across cultural and language barriers. For core architecture and compliance work, US-based or hybrid teams reduce risk.
What if a developer doesn’t know my specific EHR system?
That’s not automatically disqualifying, but it changes the timeline and risk profile. A developer with strong healthcare experience can learn a new EHR API. What matters is whether they’ve integrated with healthcare systems at all. The patterns (FHIR, HL7v2, authentication, data mapping) transfer across EHRs. A developer who’s done Epic integration can learn CentralReach. A developer who’s never touched healthcare interoperability can’t.
Sidebench Perspective
We wrote these questions because we get asked them regularly. And honestly, we think that’s how it should work. Healthcare organizations should be asking hard questions about HIPAA architecture, EHR integration experience, and measurable outcomes. The vendors who can’t answer shouldn’t be building healthcare products.
For a broader framework on evaluating healthcare technology partners (not just developers), see our partner evaluation framework. For specifics on how we approach HIPAA at the application layer, read How We Build for HIPAA.
Want to See How Sidebench Answers These Questions?
We’re happy to be evaluated against our own framework. 60+ healthcare implementations spanning 14 years. Proof points including Cortica (waitlists reduced from 6 months to 30 days; $6.7M annual platform revenue from AXON; 1 to 24 clinics across 8 states), NOCD (138M Americans covered; 1M+ therapy sessions annually; 43% symptom reduction over 12-week ERP course per peer-reviewed JMIR study), and PCIHIPAA (89% reduction in manual compliance work, acquired by Rectangle Health). Ask us anything on this list.
Use these 15 questions in your next vendor evaluation →
Cited Data Sources
- IBM Institute, Cost of a Data Breach Report 2024 ($9.77M healthcare average)
- HHS/OCR, HIPAA Breach Notification Rule (60-day requirement)
- 45 CFR 164.312, HIPAA Security Rule Technical Safeguards
About the Author
Josh Koenig leads product strategy and business development at Sidebench, a Los Angeles-based digital transformation consultancy and product studio. He works with healthcare organizations and high-growth companies to shape digital products, define scalable solutions, and guide initiatives from early discovery through proposal and delivery. His work focuses on aligning business goals, user needs, and technical strategy across areas such as patient engagement, care coordination, HIPAA-compliant platforms, and AI-enabled healthcare solutions. sidebench.com