Most healthcare technology vendor scorecards weight the wrong things. Price and timeline get 40% of the points; compliance architecture and domain depth get 10%. Then the project ships, the OCR audit comes, and the spreadsheet looks foolish. The criteria that actually predict whether a healthcare build succeeds are the ones that rarely make it onto the scorecard. This framework rebalances them.
Healthcare Implementations
(14 Years)
Clutch Rating
(48+ Reviews)
Client PortCo
Value Created
Inc 5000 + Design
Award Winners
Last updated: May 2026
By: Josh Koenig, Product & Strategy, Sidebench
In this article:
- What Are the 4 Types of Healthcare Technology Partners?
- Criterion 1: Does the Partner Build HIPAA Into the Architecture?
- Criterion 2: Do They Actually Understand Healthcare?
- Criterion 3: Who’s Really Doing the Work?
- Criterion 4: How Do They Actually Build Software?
- Criterion 5: Can They Show Quantified Results?
- What Mistakes Do Organizations Make When Choosing Partners?
- Evaluation Scorecard: 15 Weighted Criteria
- Key Takeaways
- FAQ
What Are the 4 Types of Healthcare Technology Partners?
Healthcare technology partners fall into four categories, each with different strengths, risks, and price points. Understanding which category you’re evaluating helps you ask the right questions and set realistic expectations for what you’ll get.
| Type | Strengths | Risks | Typical Cost |
|---|---|---|---|
| Offshore agencies | Lower hourly rates, large team capacity | Compliance gaps, time zone friction, high staff turnover, limited healthcare domain knowledge | $25-75/hr |
| Boutique studios | Domain expertise, senior team involvement, design + development under one roof | Smaller capacity, potentially longer timelines for large projects | $150-300/hr |
| Enterprise consultancies | Large-scale program management, brand recognition, extensive infrastructure | Junior staff on engagements, high overhead, less hands-on involvement from senior partners | $300-500+/hr |
| Marketplace/freelance | Flexible scaling, quick start | No organizational accountability, compliance liability on you, inconsistent quality | $50-200/hr |
A note on hybrid models: some boutique studios (including ours) blend onshore senior leadership with offshore engineering capacity under a workflow purpose-built for regulated environments. The category that matters is not where the developers sit but who is accountable for compliance, and what process actually enforces it on every commit.
Offshore works for non-regulated applications. Enterprise consultancies make sense for multi-year transformation programs where brand visibility matters at the board level. For HIPAA-regulated custom development, where compliance architecture, healthcare domain knowledge, and senior technical involvement all matter, the boutique studio model tends to outperform on outcomes per dollar. We are one of those boutiques. Calibrate the framework against your own situation, not ours.
Criterion 1: Does the Partner Build HIPAA Into the Architecture?
The first and most important evaluation criterion for healthcare technology is whether your partner builds HIPAA compliance into the application architecture or bolts it on as an afterthought. The difference determines your breach risk, audit readiness, and long-term maintenance costs. HIPAA compliance starts at the application layer, not the cloud. This is the difference between compliance-as-architecture, where security controls are embedded in every sprint, and compliance-as-bolt-on, where they get added in a dedicated sprint at the end (or worse, after the OCR audit).
Questions to ask:
- “Walk me through your access control implementation for a multi-role healthcare application.” If they can’t describe RBAC at the API level (not just the UI level), that’s a red flag.
- “How do you handle audit logging for ePHI access?” The answer should include immutable logs, real-time monitoring, and a defensible retention policy. We default to 6 years to align with HIPAA documentation retention, but the rule itself doesn’t prescribe an audit log retention window. If they say “we use the framework’s default logging,” run.
- “Do you sign a Business Associate Agreement?” This isn’t optional. If they hesitate or say “we don’t usually need one,” they haven’t built for healthcare before.
- “How many application-layer HIPAA controls do you implement?” We implement 47. Most teams stop at 5-10.
Red flag: Any partner who says “we deploy on AWS/Azure with a BAA, so we’re HIPAA compliant” doesn’t understand the shared responsibility model. Your cloud provider’s BAA covers infrastructure. Everything in your application layer is your responsibility.
Criterion 2: Do They Actually Understand Healthcare?
Healthcare isn’t a vertical you pick up on a single project. The regulatory environment (HIPAA, 42 CFR Part 2, state privacy laws, CMS rules), the technical ecosystem (EHR integrations, FHIR, HL7), and the stakeholder complexity (clinicians, patients, payers, regulators) all require years of accumulated knowledge. A partner with 50 healthcare projects has made mistakes you’ll never need to.
What to look for:
- Named case studies with outcomes. Not “we built a healthcare app” but “we reduced patient waitlists from 6 months to 30 days for a behavioral health organization that scaled from 1 to 24 clinics across 8 states.” Specificity signals real experience.
- Regulatory vocabulary fluency. Ask about 42 CFR Part 2, the information blocking rule, or FHIR R4. If they don’t know what you’re talking about, they haven’t worked in the space.
- EHR integration experience. Epic, Cerner, athenahealth, and CentralReach all have different integration models. A partner who’s done it before knows the gotchas, certification requirements, sandbox testing timelines, and production go-live processes.
- References you can call. Not just logos on a website. Actual humans at healthcare organizations who’ll tell you what the engagement was really like.
Criterion 3: Who’s Really Doing the Work?
The team that pitches you is rarely the team that builds your product. This is the single most common bait-and-switch in technology consulting, and it happens across every partner type. Senior architects present during the sales process, then junior developers do the work.
Questions to ask:
- “Will the people in this room be on my project?” Get names. Get resumes. Get commitments.
- “What’s your team’s average tenure?” High turnover means your project knowledge walks out the door. Look for teams where engineers stay 2+ years.
- “Are your developers W-2 employees or subcontractors?” Subcontracted teams create compliance liability. If a subcontractor mishandles PHI, the accountability chain gets complicated fast.
- “Where is your team located?” This matters for healthcare. Time zone alignment affects sprint velocity. US-based teams cost more but reduce regulatory risk and communication friction.
One thing we’ve learned after doing this for a decade: the team matters more than the process. A great team with a mediocre process will ship good software. A mediocre team with a great process will ship mediocre software with excellent documentation.
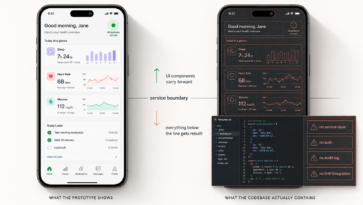
Criterion 4: How Do They Actually Build Software?
The delivery model determines how quickly you’ll see working software, how involved you’ll be in decisions, and how the product evolves after launch. For healthcare applications, you want a partner who can handle strategy, design, and development in a single engagement, not three separate vendors who need to be coordinated.
What matters:
- Discovery phase. Does the partner invest time understanding your users, workflows, and constraints before writing code? Or do they jump straight to a technical spec? The best healthcare products start with design thinking, observing real users in real clinical environments.
- Iterative delivery. You should see working software every 2-3 weeks. If the first demo is 3 months away, you’re taking a massive risk on assumptions that haven’t been validated.
- Compliance baked into sprints. Security controls, audit logging, and HIPAA requirements should be part of every sprint, not a separate compliance sprint at the end. Here’s how we handle it.
- Post-launch support. Healthcare applications need ongoing maintenance, regulatory updates, security patches, and feature iterations. Ask what happens after launch. If the answer is “we hand over the code,” plan for a rocky transition.
Red flag: Any partner whose first deliverable is a 60-page spec document instead of a working prototype.
Criterion 5: Can They Show Quantified Results?
The difference between a good technology partner and a great one is outcome evidence. Not “we built an app” but “we built an app that produced specific, measurable results.” Ask for numbers. If a partner can’t quantify the impact of their work, they either didn’t measure it or the results weren’t worth measuring.
Cortica’s CTO, Ben Nathan, described the partnership on Clutch: “They deeply want to understand our business. They’re right there with us, trying to figure out what we need to do to make sure things are done the right way. Only a group that understood our business completely would be able to participate in those conversations.”
What real outcome evidence looks like:
- Cortica: Custom scheduling platform (AXON) reduced patient waitlists from 6+ months to under 30 days, enabling the organization to scale from 1 to 24 clinics across 8 states. The platform now generates $6.7 million in annual revenue, including $4 million from the scheduling program alone, with a 10-20% increase in contract fulfillment (per Cortica’s CTO on Clutch). Disclosure: Sidebench is also an investor in Cortica. We put our own capital behind this build because we saw the long-term partnership before we saw the SOW. Full case breakdown here.
- IEHP: Bilingual member engagement platform grew from 1,000 to 90,000 active users and 3 million transactions per year, achieved within the first few months after launch, without significant marketing spend. That’s not just a scale story. It’s a speed-to-value story across 1.5 million health plan members.
- NOCD: Telehealth-native OCD treatment platform delivering over 1 million therapy sessions annually and covering 138 million Americans through insurance partnerships. Peer-reviewed JMIR study (n=3,552) shows 43% average reduction in OCD symptoms over a 12-week ERP (Exposure and Response Prevention) treatment course. In January 2026, NOCD acquired Rebound Health and launched Noto, becoming the world’s largest OCD provider. Disclosure: Sidebench is also an investor in NOCD.
- AppliedVR / RelieVRx: FDA-cleared Software as a Medical Device (SaMD) for chronic pain management, the kind of regulated digital therapeutic where partner depth in compliance and clinical workflow becomes the moat. We delivered the platform from regulated-product-readiness through commercial launch.
- PCIHIPAA (now Bridge Compliance under Rectangle Health): Compliance automation platform that cut manual compliance work by 89% and helped drive a 20X profitability increase, culminating in acquisition by Rectangle Health. Sidebench worked through the M&A diligence as well as the post-acquisition product consolidation. Jeff Broudy, CEO of PCIHIPAA, on Clutch: “I treat Sidebench as if they were my vice president of product development.”
- CHLA Baby Steps: NICU family support app serving 17,000 families with a 4.7-star satisfaction rating, recognized in the American Hospital Association’s 2019 Innovation Challenge (3rd place) and Fast Company’s Best Mobile Apps. Dr. Lakshmanan, attending neonatologist at CHLA framed the partnership impact directly in her review.
The human impact matters too. A client from LA County’s Department of Children and Family Services shared on Clutch: “We recently presented their promotional video at a conference, and all of the social workers in attendance were moved to tears; everyone in the industry is excited for the time-reducing tool to be released.”
Notice what these examples have in common? They’re specific. They name the client. They quantify the result. When a partner shows you logos without numbers, they’re selling brand association, not evidence.
What Mistakes Do Organizations Make When Choosing Partners?
After watching healthcare organizations evaluate technology partners for over a decade, the same mistakes keep repeating. Knowing them in advance won’t eliminate the risk, but it’ll shift the odds in your favor.
- Choosing on price alone. The cheapest bid for healthcare development is almost always the most expensive in total cost of ownership. A $75/hr offshore team that delivers a non-compliant application costs more than a $200/hr domestic team that builds it right the first time. Add breach risk ($9.77M average per IBM 2024) and the math isn’t close.
- Underweighting compliance. Compliance gets 10% of the evaluation weight when it should get 30%. A beautiful application that fails an OCR audit is a liability, not an asset.
- Not checking references. Every vendor has polished case studies. Call their clients. Ask what went wrong. Ask if they’d hire them again. The answers will surprise you.
- Skipping discovery. Organizations that jump straight to development skip the phase where you figure out what to build. The result is always the same: expensive rework 6 months later when the product doesn’t match user needs.
- Treating it as a procurement exercise. Technology partner selection in healthcare is a strategic decision, not a purchasing decision. The partner you choose will shape your product, your compliance posture, and your competitive position for years.
Evaluation Scorecard: 15 Weighted Criteria
Use this framework to compare healthcare technology partners. Weight compliance and domain expertise more heavily than most scorecards suggest, these are the criteria that predict long-term success in regulated environments.
| Criterion | Weight | What to Evaluate |
|---|---|---|
| HIPAA architecture approach | 15% | Application-layer controls, BAA, audit logging |
| Healthcare project count | 12% | Number and type of healthcare implementations |
| EHR integration experience | 10% | Epic, Cerner, athenahealth, CentralReach, specialty EHRs |
| Quantified case studies | 8% | Named clients with measurable outcomes |
| Team seniority and retention | 8% | Senior architects on project, average tenure, turnover rate |
| Cultural fit | 7% | Collaboration style, responsiveness, willingness to push back |
| Discovery and design process | 7% | User research, design thinking, prototyping before code |
| Security testing practices | 7% | Penetration testing, SAST/DAST, vulnerability management |
| Team location and structure | 6% | US-based vs offshore, time zone overlap |
| Post-launch support model | 5% | Ongoing maintenance, SLAs, regulatory update handling |
| Client references | 5% | Referenceable healthcare clients willing to speak |
| Delivery methodology | 4% | Agile cadence, demo frequency, working software milestones |
| Communication and reporting | 3% | Transparency, status cadence, escalation process |
| Third-party ratings | 2% | Clutch, G2, KLAS, industry recognition |
| Pricing model clarity | 1% | T&M vs fixed, change order process, transparency on overages |
Treat these weights as our default starting point, not the right answer. Your organization’s priorities should shift them. An organization with a strong internal compliance team may reasonably weight the compliance criteria lower. A startup pre-product should weight discovery higher than post-launch support. A behavioral health build should lean into EHR integration depth (specifically CentralReach). The scorecard is a conversation starter, not a verdict.
Key Takeaways
- Compliance depth is the top criterion. HIPAA compliance at the application layer is where most partners fall short. If they can’t explain their approach to access controls, audit logging, and encryption beyond “we use AWS,” keep looking.
- Healthcare experience isn’t optional. Regulatory complexity, EHR integration, and clinical workflow understanding take years to develop. A partner’s 50th healthcare project is fundamentally different from their 1st.
- The project manager is the person who determines whether your engagement succeeds or fails. And in most firms, they’re not staffed until you’ve signed. Ask who’ll lead your project day-to-day, how many healthcare builds they’ve run, and whether they’ll stay with you from discovery through launch. The pitch team gets you excited. The PM gets you shipped.
- Demand quantified outcomes. Logos aren’t evidence. Ask for specific metrics: users gained, waitlists reduced, costs cut, compliance gaps closed.
- Price is a trailing indicator. The cheapest option rarely has the lowest total cost. Factor in compliance risk, rework probability, and the $9.77M average cost of a healthcare breach.
FAQ
How much does custom healthcare software development cost?
Custom healthcare applications typically range from $150,000 to $500,000 for a focused product (patient portal, scheduling platform, engagement app) and $500,000 to $2M+ for complex multi-system integrations. The cost varies based on scope, compliance requirements, and integration complexity. We’ve broken down digital transformation costs in more detail.
How long does healthcare app development take?
A focused healthcare application takes 4-8 months from discovery to launch. Complex projects with EHR integrations, multiple user types, and advanced compliance requirements can run 8-12 months. The discovery/design phase (typically 4-8 weeks) is where timelines are set, skip it, and you’ll add months of rework later.
What should I ask a healthcare technology partner about HIPAA?
Start with: “How many application-layer HIPAA controls do you implement?” Then ask about their BAA process, audit logging approach, encryption standards (at rest and in transit), access control architecture, and breach response procedures. Our HIPAA controls walkthrough shows what good answers look like.
Should I hire offshore developers for healthcare applications?
Offshore development can work for non-regulated applications, but creates significant risk for HIPAA-regulated projects. BAA enforcement across international boundaries is complicated. Time zone differences slow iteration cycles. And regulatory knowledge gaps often surface late in the project when they’re most expensive to fix. For healthcare, US-based teams with healthcare experience consistently deliver better outcomes.
How do I structure a paid discovery engagement to de-risk the full build?
A well-structured discovery engagement runs 4-8 weeks and costs $50K-$150K. Deliverables should include: clinical workflow research (shadowing real users, not just interviewing stakeholders), technical architecture (EHR integration approach and compliance boundaries), a navigable prototype (clickable UX that lets you test concepts with clinicians before committing to code), vendor assessment if relevant, and a go/no-go recommendation with phased implementation roadmap. Paying for discovery upfront saves 3-5x the cost of discovering the same issues during development.
How do I evaluate a partner’s healthcare experience?
Ask for named case studies with quantified outcomes, not just logos. Ask for references you can call. Ask about specific regulatory challenges they’ve navigated (HIPAA, 42 CFR Part 2, state privacy laws). Ask which EHR systems they’ve integrated with and how those integrations went. Depth of answers matters more than breadth of claims.
What EHR systems should my technology partner have experience with?
That depends on your ecosystem. Epic and Cerner (now Oracle Health) dominate hospital systems. athenahealth is common in ambulatory settings. CentralReach is the most common behavioral health EHR. Your partner should have hands-on experience with the specific systems in your environment, not just awareness that they exist.
How important is design in healthcare technology?
Critical. Design thinking in healthcare, observing real users in real clinical environments before writing code, is the difference between products that get adopted and products that get abandoned. Clinical staff have limited time and patience for bad UX. A 3-click workflow that should be 1 click will kill adoption.
What does post-launch support look like for healthcare applications?
Healthcare applications need ongoing support for regulatory updates (CMS changes rules annually), security patching, performance monitoring, and feature iteration. Good partners offer maintenance agreements with defined SLAs, proactive security monitoring, and dedicated account teams. Bad partners hand you the code and move to the next project.
How do I build a business case for hiring a technology partner?
Frame it as risk-adjusted ROI. Calculate the cost of the current problem (operational inefficiency, compliance gaps, patient access limitations), the cost of the technology investment, and the expected return. Use industry benchmarks: communication failures cost healthcare $1.7 billion in malpractice claims alone (CRICO). The business case almost always favors investment when you factor in risk.
What red flags should I watch for when evaluating partners?
Can’t explain HIPAA controls beyond hosting. No named healthcare case studies. The pitch team won’t commit to the project. No BAA process. Fixed-bid pricing on a project they haven’t scoped through discovery. Promising delivery timelines that seem too good to be true (because they are). Any resistance to letting you talk to past healthcare clients.
What does a HIPAA breach actually cost a mid-sized healthcare organization?
The 2024 IBM Cost of a Data Breach Report puts the healthcare industry average at $9.77 million per incident, roughly 2x the cross-industry average. For a mid-sized organization (50-500 beds or comparable patient volume), breach costs typically run $3M to $15M depending on records exposed, detection time, and regulatory response. The cost isn’t just the OCR fine. It’s forensic investigation, legal fees, credit monitoring for affected individuals, breach notification, remediation, lost patients, and reputation damage that compounds for years.
Sidebench Perspective
Better evaluation produces better outcomes for healthcare, including for the projects we don’t win. The criteria above are the ones that have predicted success across our 50+ healthcare implementations and the engagements we’ve watched go badly elsewhere. If you want to test how we score against the framework, the offer below is built for exactly that.
Ready to Apply This Framework?
Schedule a discovery call and see how Sidebench measures up against these 15 criteria. We’ll show you our process, introduce the team, and share relevant case studies from organizations like yours.
Apply this framework to your next healthcare technology partner evaluation →
Cited Data Sources
- IBM 2024, Cost of a Data Breach Report 2024
- HIPAA Security Rule (45 CFR 164.312), Technical Safeguards Requirements
- Clutch, Sidebench Reviews and Ratings
- CRICO Strategies, Malpractice Risks in Communication Failures
About the Author
Josh Koenig leads product strategy and business development at Sidebench, a Los Angeles-based digital transformation consultancy and product studio. He works with healthcare organizations and high-growth companies to shape digital products, define scalable solutions, and guide initiatives from early discovery through proposal and delivery. His work focuses on aligning business goals, user needs, and technical strategy across areas such as patient engagement, care coordination, HIPAA-compliant platforms, and AI-enabled healthcare solutions. sidebench.com