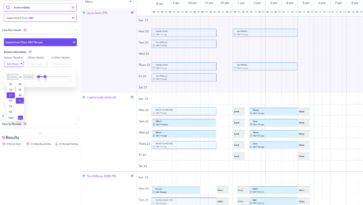
A multi-site Applied Behavior Analysis (ABA) therapy provider came to us after their growth stalled at 8 clinics. Not because demand dropped – their waitlist was 4 months long. The bottleneck was technology: scheduling was manual, intake forms were paper-based, and patient data lived in three disconnected systems. Every new clinic multiplied the chaos rather than the capacity.
They had an Electronic Health Record (EHR). They had a scheduling system. They had a patient portal. None of them talked to each other, and none of them were built for behavioral health workflows.
This pattern repeats across the $89 billion behavioral health market. The sector is growing faster than almost any other in healthcare – ABA therapy visit volume increased 267% between 2019 and 2024 (Clarify Health, 2024). Private equity is flooding in. Multi-site expansion is the mandate.
But the technology infrastructure hasn’t kept pace. Only 6% of behavioral health facilities use electronic health records – compared to over 80% of hospitals (MACPAC, 2022). The vast majority operate on paper, spreadsheets, and manual workarounds – which means every new location inherits the inefficiencies of the last.
This guide covers the technology decisions that determine whether a behavioral health organisation scales or stalls. Not generic “digital transformation” – specific to multi-site behavioral health (BH) operations, ABA scheduling complexity, intake automation, and payer compliance.
Healthcare Implementations
Platform Users Scaled
Compliant Architecture
Client Value Created
Last updated: February 2026
By: Kevin Yamazaki, Partner, CEO at Sidebench
- Why do generic EHRs fail behavioral health organizations?
- What are the 5 technology inflection points for scaling?
- How does scheduling become the first bottleneck?
- Why is intake where most patients are lost?
- When should you build custom technology vs. buy off-the-shelf?
- What does this actually cost?
- Case study comparison: Cortica, NOCD, LEARN
- What should you look for in a technology partner?
- 5 warning signs your technology can’t scale
- Frequently Asked Questions
- Key Takeaways
Why do generic EHRs fail behavioral health organizations?
Generic EHRs are built for encounter-based medicine – a patient arrives, receives treatment, and leaves. Behavioral health is session-based, requiring ongoing scheduling across multiple providers, complex authorization workflows, and documentation formats that traditional EHRs don’t support. This fundamental mismatch is why workflow fit is consistently the top EHR selection criterion for behavioral health providers (KLAS, 2024).
Epic and Cerner dominate the hospital EHR market. But their behavioral health modules are adaptations, not purpose-built systems. They were designed for acute care – emergency department visits, surgeries, inpatient stays. This is why specialized BH EHRs like CentralReach, TherapyNotes, SimplePractice, and Valant exist – and why even those often require custom layers for multi-site scaling.
Behavioral health requires something fundamentally different:
Session-based vs. encounter-based models
A behavioral health patient might see multiple providers across multiple sessions per week, each with different authorization requirements and documentation standards. Traditional EHRs expect one encounter = one visit = one billing event. Behavioral health is more complex.
| Dimension | Traditional EHR | Behavioral Health Reality |
|---|---|---|
| Visit frequency | Episodic (annual, acute) | Regular (2-5 sessions/week) |
| Provider relationship | Multiple providers per visit | Single provider over months/years |
| Scheduling complexity | Book appointment, confirm | Match patient to provider, authorization, recurring patterns |
| Documentation | Structured templates | Session notes, progress tracking, treatment plans |
| Telehealth | Add-on module | Native requirement |
| Authorization | Per-episode | Per-session, per-service, per-payer |
42 CFR Part 2 complexity
Behavioral health records are subject to additional federal privacy requirements beyond HIPAA. 42 CFR Part 2 restricts disclosure of substance use disorder (SUD) treatment records more strictly than general medical records. Many generic EHRs cannot segment SUD records appropriately, creating compliance risk every time data is shared.
What are the 5 technology inflection points for scaling?
Scaling from 1 clinic to 50 requires solving five sequential technology problems:
- Scheduling optimization
- Intake automation
- EHR integration
- Multi-site data consistency
- Layer compliance
Organizations that address these in order scale smoothly; those that skip ahead encounter compounding bottlenecks.
Each inflection point represents a moment where manual processes break down and technology becomes essential – not optional.
Inflection Point 1: Scheduling at Scale
At 1-3 clinics, a clinical coordinator can manage scheduling manually. At 10+ locations, this becomes impossible. You need algorithmic matching:
patient needs → provider availability → authorization status → location constraints → recurring pattern optimization.
Case study: Cortica built the AXON platform to solve exactly this. Their 6-month patient waitlist dropped to under 30 days. They scaled from 1 clinic to 16. Valuation increased by $200M.
Inflection Point 2: Intake Automation
Paper intake forms, faxed referrals, and manual data entry create a 30% abandonment rate before patients even see a provider. Digital intake – with pre-population, eligibility verification, and automatic EHR population – recaptures this lost demand.
Case study: LEARN Behavioral automated their intake process and reduced time-to-first-appointment while improving conversion rates.
Inflection Point 3: EHR Integration Without Rip-and-Replace
Most organizations can’t (and shouldn’t) replace their EHR. They need integration: scheduling systems that read from and write to the EHR, intake tools that populate patient records, and analytics that pull from multiple data sources.
Inflection Point 4: Multi-Site Data Consistency
When each clinic operates its own systems, you lose visibility. Clinical leadership can’t see aggregate waitlists, compare provider productivity, or identify bottlenecks across locations. A unified data layer – even if the underlying systems differ – is essential.
Inflection Point 5: Payer Compliance and Authorization
Each payer has different authorization requirements, documentation standards, and reimbursement rules. At scale, tracking this manually leads to denied claims and delayed payments. Automated authorization tracking and documentation compliance become essential.
| Inflection Point | Trigger | Technology Solution |
|---|---|---|
| Scheduling | 3+ clinics | Algorithmic patient-provider matching |
| Intake | 30%+ abandonment | Digital intake with eligibility verification |
| EHR integration | Multiple systems | API-based integration layer |
| Multi-site data | 5+ locations | Unified analytics platform |
| Payer compliance | Multi-payer | Automated authorization tracking |
How does scheduling become the first bottleneck?
Scheduling is the first bottleneck because behavioral health scheduling is inherently more complex than general medical scheduling. A single ABA patient might require 10-25 hours of therapy per week, matching specific therapist credentials to specific patient needs, across multiple days and locations. Manual scheduling can’t optimize this at scale.
Consider the constraints a behavioral health scheduler must balance:
- Patient needs – diagnosis, treatment plan, language, location preference
- Provider qualifications – credentials, specializations, caseload capacity
- Authorization status – which services are approved, how many hours remain
- Location availability – room availability, equipment, accessibility
- Recurring patterns – behavioral health requires consistency, not one-off appointments
- Travel time – if providers serve multiple locations, routing matters
At 3 clinics with 10 providers, a skilled coordinator might manage this. At 10 clinics with 40 providers, it’s impossible without technology.
The Cortica Solution: AXON Platform
When Cortica – a leading autism and developmental health organization – faced this challenge, they had a 6-month patient waitlist. Families were waiting half a year for treatment that early intervention research shows is most effective when started immediately.
The AXON platform Sidebench built does algorithmic matching: patient requirements are matched to provider availability across all clinic locations, optimizing for minimum wait time and maximum care continuity. Results:
- Waitlist reduction: 6 months → under 30 days
- Clinic expansion: 1 clinic → 16 clinics
- Valuation impact: $200M increase
- Appointment volume: 1M+ patient appointments annually
Why is intake where most patients are lost?
Intake is where most patients are lost because the gap between initial inquiry and first appointment is where complexity creates friction. Paper forms, phone tag, eligibility confusion, and authorization delays combine to create a 30% average abandonment rate in behavioral health. Every lost patient is lost revenue and – more importantly – a family that doesn’t get care.
The typical behavioral health intake process looks like this:
- Family calls or submits web inquiry
- Staff calls back (phone tag begins)
- Forms are mailed or faxed
- Forms are returned, manually entered
- Eligibility is verified manually
- Authorization is requested from payer
- Authorization is received (days to weeks later)
- Appointment is scheduled
- Patient finally receives care
At each step, there’s an opportunity for delay, error, or abandonment. Families dealing with a child’s behavioral health needs are often overwhelmed. If the process is difficult, they disappear.
Digital Intake Transformation
Modern intake automation addresses each friction point:
| Traditional Intake | Automated Intake |
|---|---|
| Paper forms mailed/faxed | Digital forms on any device |
| Manual data entry | Auto-population into EHR |
| Phone-based eligibility verification | Real-time eligibility check |
| Manual authorization request | Automated authorization submission |
| Days-to-weeks wait for status | Real-time status dashboard |
| No visibility into drop-off | Conversion funnel analytics |
Case study: LEARN Behavioral implemented automated intake with real-time eligibility verification, reducing the inquiry-to-appointment timeline and improving conversion. When families can complete intake on their phone immediately – rather than waiting for paper forms – completion rates increase significantly.
When should you build custom technology vs. buy off-the-shelf?
Build custom when your workflow is a competitive advantage, when off-the-shelf solutions require so much customization they approach custom cost, or when integration requirements exceed what standard products offer. Buy when the functionality is commodity, when your workflow matches industry standard, and when speed-to-deploy matters more than differentiation.
This isn’t an all-or-nothing decision. Most behavioral health organizations end up with a hybrid: off-the-shelf EHR for core clinical documentation, custom scheduling for their specific optimization needs, integrated intake for patient experience.
Decision Framework
| Factor | Build Custom | Buy Off-the-Shelf |
|---|---|---|
| Workflow uniqueness | Your process is your competitive advantage | Your process matches industry standard |
| Integration complexity | Multiple systems must work together seamlessly | Single-system or standard integrations |
| Vendor customization | Vendor quotes 6+ months of customization | Works mostly out of the box |
| Total cost | Build + maintain < License + customize | License + customize < Build + maintain |
| Time to value | Can wait 6-12 months for right solution | Need something working in 90 days |
| Long-term ownership | Want to own the IP, control the roadmap | Prefer vendor manages updates |
| Regulatory requirements | Unusual compliance needs (42 CFR Part 2, state-specific) | Standard HIPAA requirements |
The Hybrid Approach
The most successful behavioral health organizations we’ve worked with use a hybrid model:
- EHR: Off-the-shelf (often specialized BH EHR like TherapyNotes, SimplePractice, or Qualifacts)
- Scheduling: Custom (the optimization complexity justifies custom)
- Intake: Custom or heavily configured (patient experience differentiation)
- Analytics: Custom (unified view across systems)
- Patient Portal: Depends on EHR and differentiation needs
What Does This Actually Cost?
CTOs and COOs need budget reality, not vague ranges. Here’s what behavioral health technology investments typically look like:
| Solution Type | Initial Investment | Ongoing (Annual) | Time to Value |
|---|---|---|---|
| Off-the-shelf BH EHR | $10K-$50K setup | $500-$2K/month | 2-4 months |
| Custom scheduling platform | $150K-$400K | $30K-$60K maintenance | 6-9 months |
| Intake automation | $75K-$200K | $15K-$30K maintenance | 4-6 months |
| Full platform (scheduling + intake + analytics) | $300K-$750K | $50K-$100K maintenance | 9-12 months |
The question isn’t “can we afford this?” – it’s “can we afford not to, given what manual processes cost at scale?”
What does success look like? Case Study Comparison
Three behavioral health organizations, three different starting points, three technology-enabled transformations:
Cortica: From Waitlist Crisis to Scaled Growth
| Before | After |
|---|---|
| 6-month patient waitlist | <30 day waitlist |
| 1 clinic | 16 clinics |
| Manual scheduling across disconnected systems | AXON platform with algorithmic optimization |
| Limited visibility into capacity | Real-time capacity management |
| Valuation: Pre-growth | Valuation: +$200M |
Key technology: Custom scheduling platform integrating multiple EHR and billing systems, algorithmic patient-provider matching, multi-location capacity optimization.
NOCD: From Startup to Category Leader
| Before | After |
|---|---|
| $5M valuation | $150M+ valuation |
| Manual therapist matching | Algorithmic therapist-patient matching |
| Basic telehealth | Native telehealth with ERP integration |
| Limited outcome tracking | 40%+ OCD symptom reduction in 3 weeks |
Key technology: Purpose-built OCD treatment platform, not adapted from general mental health tools. Telehealth as core experience, not add-on.
LEARN Behavioral: Intake as Competitive Advantage
| Before | After |
|---|---|
| Paper intake forms | Digital intake on any device |
| High abandonment | Improved conversion |
| Manual eligibility verification | Automated verification |
| Weeks to first appointment | Reduced time-to-first-appointment |
Key technology: Automated intake workflow with real-time eligibility verification and EHR integration.
What should you look for in a technology partner?
Look for behavioral health-specific experience, not just healthcare experience. HIPAA + 42 CFR Part 2 compliance. ABA workflow understanding. EHR integration capability. And measurable outcomes from previous implementations – not just “we built an app.”
Evaluation Criteria
| Criterion | What to Ask | Red Flag |
|---|---|---|
| BH-specific experience | “Show me behavioral health projects you’ve completed.” | Only general healthcare experience |
| Compliance depth | “How do you handle 42 CFR Part 2 in your architecture?” | “We’re HIPAA compliant” (incomplete answer) |
| Workflow understanding | “Walk me through how you’d approach ABA scheduling.” | Generic scheduling solution proposed |
| Integration capability | “How would you integrate with our existing EHR?” | Rip-and-replace recommendation |
| Outcome evidence | “What measurable outcomes did your clients achieve?” | “We built a great product” (no metrics) |
| Team structure | “Who would actually work on our project?” | Offshore team with no healthcare experience |
The “Too Complex” Test
If your technology partner can’t explain how they’d handle these three scenarios, they don’t understand behavioral health:
- Multi-payer authorization: Patient has two insurance plans with different ABA authorization limits. How does your system track both?
- Provider credential matching: Patient needs Spanish-speaking, pediatric-specialized ABA therapist with RBT certification. How does scheduling find the match?
- Telehealth/in-person hybrid: Same patient, some sessions in-clinic, some telehealth. How does documentation flow correctly to each billing code?
5 Warning Signs Your Technology Can’t Scale
Before you hit a growth wall, watch for these red flags:
- Scheduling takes longer as you grow – If adding a clinic means hiring another coordinator, your scheduling doesn’t scale. It should get easier with more locations, not harder.
- Intake abandonment is rising – Track inquiry-to-first-appointment conversion. If it’s dropping as volume increases, your intake process can’t handle the load.
- Staff spend more time on workarounds than work – When clinical staff create their own spreadsheets, shadow systems, or manual tracking outside the EHR, your technology has gaps.
- You can’t answer basic capacity questions – “How many patients could we serve next month if we hired 3 more therapists?” If this takes a week to answer, you lack visibility.
- New locations inherit old problems – Each clinic launch should be faster and cleaner than the last. If location #8 is as chaotic as location #2, your systems aren’t maturing.
If you recognize three or more of these, technology is constraining your growth – not enabling it.
Frequently Asked Questions
What is behavioral health technology?
Behavioral health technology encompasses software and digital tools specifically designed for mental health, substance use disorder, and developmental health organizations. This includes EHR systems, scheduling platforms, telehealth tools, intake automation, outcome measurement, and payer compliance systems – all built for session-based care models rather than traditional encounter-based healthcare.
Why is behavioral health EHR adoption so low?
Fewer than 25% of behavioral health facilities report exclusive EHR use because generic healthcare EHRs don’t fit behavioral health workflows. Session-based documentation, complex authorization requirements, and 42 CFR Part 2 compliance needs require specialized solutions that mainstream EHR vendors haven’t prioritized.
How much does ABA scheduling software cost?
ABA scheduling software costs vary widely: off-the-shelf solutions range from $500-$2,000/month, while custom-built platforms typically cost $150K-$500K for development plus ongoing maintenance. The right choice depends on organization size, workflow complexity, and whether scheduling optimization is a competitive differentiator.
What is 42 CFR Part 2 and why does it matter?
42 CFR Part 2 is a federal regulation providing additional privacy protections for substance use disorder treatment records beyond HIPAA. It restricts how SUD records can be disclosed and requires specific consent procedures. Technology systems must be able to segment and control SUD data separately from general medical records.
How do you integrate behavioral health systems with hospital EHRs?
Integration typically uses HL7 FHIR APIs for data exchange, middleware for translation between systems, and careful mapping of behavioral health-specific data elements. The key is maintaining data consistency while respecting the different documentation and workflow requirements of each system.
What causes high patient abandonment in behavioral health intake?
High abandonment stems from process friction: paper forms, phone tag, manual verification, and long wait times between inquiry and first appointment. Families dealing with behavioral health needs are often overwhelmed; complex intake processes cause them to disengage before receiving care.
How does telehealth change behavioral health technology requirements?
Telehealth shifts requirements from “add-on” to “core.” Video platform, patient scheduling, therapist availability, documentation, billing codes, and outcome measurement must all work seamlessly in a telehealth-first model. Platforms originally designed for in-person care often struggle with this integration.
What’s the difference between ABA scheduling and general medical scheduling?
ABA scheduling must optimize for 10-25 hours of therapy per week per patient, match specific therapist credentials to patient needs, track remaining authorized hours, and maintain consistency for patients who benefit from the same therapist over time. General scheduling books single appointments without these constraints.
How do behavioral health organizations track outcomes?
Outcome tracking uses standardized assessment instruments (PHQ-9, GAD-7, YBOCS for OCD, etc.) administered at regular intervals, with results integrated into the EHR. The key is consistent collection across all patients and providers, which requires technology to prompt assessments and aggregate results.
Should behavioral health organizations use specialized BH EHRs or major platforms like Epic?
Specialized BH EHRs (TherapyNotes, SimplePractice, Valant, Qualifacts) are generally better fits for standalone behavioral health organizations. Epic or Cerner may make sense for BH departments within larger health systems. The decision depends on integration requirements, budget, and how much customization you’ll need.
How long does it take to implement custom behavioral health technology?
Custom platform development typically takes 6-12 months from discovery to launch, depending on scope. A focused scheduling optimization might take 4-6 months; a comprehensive platform including intake, scheduling, documentation, and analytics might take 9-12 months. Speed depends on clarity of requirements and decision-making velocity.
What should a behavioral health technology RFP include?
RFP must-haves: specific workflow requirements (not generic features), integration requirements with existing systems, compliance requirements including 42 CFR Part 2, outcome expectations (not just deliverables), and questions about vendor’s behavioral health-specific experience.
Key Takeaways
- Generic EHRs fail behavioral health – They’re built for encounter-based medicine, not session-based care. This is one of the most common health tech challenges we see – workflow mismatch creates operational friction at every step.
- Scheduling is the first bottleneck – At 3+ clinics, manual scheduling breaks. Algorithmic optimization isn’t a nice-to-have; it’s essential for reducing waitlists and maximizing capacity.
- Intake determines who gets care – 30% of potential patients abandon before first appointment. Digital intake automation recaptures this lost demand.
- Build vs. buy depends on strategy – If workflow optimization is your competitive advantage, build custom. If it’s commodity functionality, buy off-the-shelf.
- 42 CFR Part 2 isn’t optional – Substance use disorder records have stricter requirements than HIPAA. Combined with HIPAA application layer compliance, technology must handle both or you’re at compliance risk.
- Behavioral health-specific experience matters – General healthcare experience isn’t enough. Ask for BH-specific case studies, workflow understanding, and 42 CFR Part 2 compliance evidence.
Ready to Scale?
Scaling a behavioral health organization? We’ve built technology for organizations from early-stage startups to 16-clinic operations processing 1M+ appointments annually.
Cited Data Sources
- SUD Treatment Dropout Meta-analysis – Meta-analysis of SUD treatments: “average dropout rate across all studies was 30.4%”
- PMC Dropout Study – PMC study: “projected cumulative dropout was estimated to be close to 30%”
- 42 CFR Part 2 Final Rule – Fact Sheet 42 CFR Part 2 Final Rule
- Behavioral Health EHR Adoption – 6% of Behavioral Health Facilities Use EHRs – Behavioral Health Business
About the Author
Kevin Yamazaki, Partner and CEO at Sidebench, has led behavioral health technology implementations for organizations including Cortica, NOCD, and LEARN Behavioral. With expertise spanning ABA scheduling optimization, intake automation, and behavioral health platform development, he focuses on helping organizations scale without sacrificing clinical quality. sidebench.com