Most longevity technology investments underperform, not because the market is wrong but because teams skip the product strategy work that determines whether a platform scales or stalls. The opportunity is real ($93 billion by 2027, 7.5% CAGR), but health systems, concierge clinics, and consumer wellness platforms keep making the same avoidable mistakes at the business case stage. This is a framework for executives who need to justify a longevity technology investment to their board, pick the right implementation approach, and avoid the mistakes that kill ventures before they reach patients. Not a primer on longevity science.
Healthcare Implementations
(14 Years)
Client PortCo
Value Created
Clutch Rating
(48+ Reviews)
Last updated: May 2026
By: Kevin Yamazaki, Partner, CEO at Sidebench
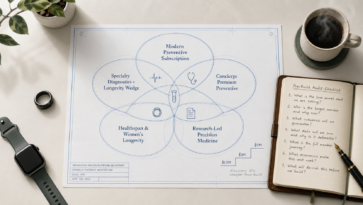
The Three Longevity Market Segments You’re Actually Competing In
Three distinct segments make up the longevity technology market, each with a different technology stack, business model, and go-to-market approach. Getting the segment wrong at the business case stage means building the wrong product entirely.
Segment 1: Health System Preventive Care Arms. Traditional hospital systems launching longevity-focused product lines. Think a regional hospital creating a consumer wellness app to extend patient relationships beyond episodic care. These projects live inside existing compliance frameworks and EHR ecosystems, which means Epic or Athena integration isn’t optional. It’s the first technical constraint you’ll hit.
Segment 2: Concierge and Clinical Longevity Practices. Cardio-cognitive clinics, functional medicine practices, and multisite concierge operations building patient-facing digital companions. The technology challenge here isn’t scale, it’s clinical workflow integration. Every platform needs to pull from and push to an EMR while supporting the high-touch care model these clinics sell.
Segment 3: Direct-to-Consumer Longevity Platforms. Membership-based wellness products competing for consumer attention and retention. The technology priorities flip: conversion optimization, brand experience, and growth mechanics matter more than clinical integration. But HIPAA still applies the moment you’re handling health data.
| Health System Arms | Concierge Clinics | DTC Platforms | |
|---|---|---|---|
| Primary tech challenge | Data quality and engineering + EHR integration at scale | Clinical workflow + EMR | Conversion + retention |
| Compliance burden | High (existing frameworks) | Medium (smaller scale) | Variable (data-dependent) |
| Revenue model | High-margin preventive care, cash-pay wellness, employer contracts | Membership + fee-for-service | Subscription + upsell |
| Typical tech investment | $200K-$1M+ | $100K-$400K | $150K-$500K |
| Critical success metric | Patient panel growth | Provider adoption rate | Member growth + LTV |
Why Most Longevity Tech Investments Fail Before Launch
Longevity technology projects don’t fail because the technology is hard. They fail because leadership teams skip the product strategy work that de-risks the investment before development begins. Three patterns show up repeatedly across failed projects.
They skip product strategy and technical validation. Teams jump from “we need an app” to hiring developers. Nobody validated whether the product concept solves a problem patients will pay for, or whether providers will adopt it. A 6-week discovery and solution design engagement that produces a user-validated navigable prototype, technical architecture, and go/no-go roadmap costs a fraction of a failed build. We’ve run these for a major regional hospital system, a cardiocognitive longevity clinic, and a national radiology AI provider. In each case, discovery surfaced risks, EHR integration gaps, workflow mismatches, compliance blind spots, that would’ve cost 10x more to find during development.
They underestimate EHR integration complexity. “We’ll just connect to Epic” is the most expensive sentence in health tech. Integration isn’t a feature you bolt on at the end. It’s an architectural decision that shapes your entire data model, authentication flow, and deployment timeline. We’ve seen organizations budget 3 months for Epic integration and spend 18. The projects that succeed treat EHR integration as the first constraint, not the last feature.
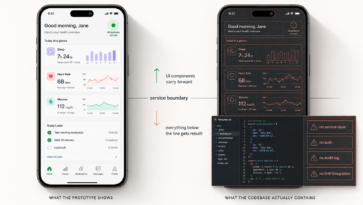
They build for launch, not for scale. A longevity platform that works for 500 patients and breaks at 5,000 is a product strategy problem wearing a technology costume. We’ve helped clients grow platforms from 35,000 to more than 2 million patient appointments in a single year, and from zero to 90,000 weekly active users in six months. The architecture decisions made in month one determined whether that growth was possible.
The Board-Ready Business Case Framework
Your board cares about three things when evaluating a longevity technology investment: how big is the opportunity, what does it cost, and what’s the risk if you don’t move. Structure your business case around these three sections and you’ll get past the first conversation.
Section 1: Market Opportunity (Make It Specific)
Don’t cite the $93 billion global market and call it a day. Boards see through that. Instead:
- Bulletproof your addressable market definition. The lazy TAM calculation doesn’t survive a real board conversation. Build the analysis through two lenses, conservative and optimistic, each with math and assumptions that hold up to five levels of “why” and “why not.” Start from your existing reach and patient base, not a topline population number. If you’re a health system in Southern California, the honest addressable market is the slice of your service-area panel who would actually use and pay for a preventive care platform under each lens. For one regional hospital system, this analysis produced a 10x-25x patient scale target for their web relaunch, a number the board could defend because the assumptions behind it were pressure-tested, not aspirational.
- Show the competitive gap. Who else serves this patient population with longevity technology? Most health systems will find the answer is “nobody with clinical credibility.”
- Quantify the retention opportunity. Patients who engage with a health system’s longevity platform don’t leave for a DTC competitor. Model the lifetime value difference between a retained patient and one who churns. And model LTV-to-CAC. In the early stages of a longevity offering, acquisition costs are low (existing patients, employer referrals, practice panel) and lifetime value is years, not months. The ratio tends to be unusually favorable, and boards respond to that math.
Section 2: Investment Structure (Phase It)
Boards don’t approve $2 million lump sums for unproven ventures. They approve phased investments with clear go/no-go gates.
| Phase | Duration | Investment | Deliverables | Go/No-Go Gate |
|---|---|---|---|---|
| Discovery & Solution Design | 4-8 weeks | $50K-$150K | User-validated navigable prototype, technical architecture, EHR integration risk map, data model & integration testing plan, compliance gap analysis, RACI sign-off, phased roadmap | Does the concept survive contact with real users and real EHR constraints? |
| MVP development | 12-20 weeks | $200K-$500K | Working platform, core integrations, initial user cohort | Does the product hit target adoption within 90 days? |
| Scale + optimization | Ongoing | $100K-$300K/yr | Feature expansion, integration deepening, growth mechanics | Does unit economics improve quarter over quarter? |
Early-stage product strategy is where most of the risk must be eliminated. A well-scoped $100K strategy and design engagement that produces a user-validated prototype, technical architecture, and go/no-go decision saves you from a $500K build that nobody uses.
Section 3: Risk Register (Be Honest)
Boards respect executives who name risks rather than hide them. Here are the ones that actually matter:
| Risk | Probability | Impact |
|---|---|---|
| EHR integration timeline overrun | High | High |
| AI features crossing from “clinical decision support” into FDA-regulated Software as a Medical Device (SaMD) without the team realizing it | Medium | Very High |
| Training or fine-tuning AI models on PHI without proper de-identification, triggering HIPAA minimum necessary and use-limitation violations | Medium | High |
| Wearable data access gates: device manufacturers restricting/repricing API access after your platform depends on their data | Medium | Medium |
| Provider adoption resistance | High | Medium |
| Consumer retention below breakeven | Medium | High |
| Regulatory shifts in health data handling | Low | High |
Mitigation pattern that works across all seven risks: pull in domain experts early; test and validate integrations with a skeptical eye; understand constraints before designing around them; build internal champions who understand the product vision; and stress-test the largest risk points outside your direct control, ideally with someone who’s been burned by those points before. We’ve built technical and compliance blueprints for HIPAA-managed AI workflows with explicit integration boundaries, ingestion and storage patterns, and admin workflows, so AI features can be productized while protecting clinical trust.
What Longevity Technology Actually Needs to Do
Every longevity platform, whether it’s for a large health system, a growing concierge clinic brand, or a DTC platform, needs five core technical capabilities. Missing any one of them creates a gap that compounds as you scale, and the cost of retrofitting compounds after launch.
Device and Wearable Data Ingestion
Longevity platforms live on data. Apple Health, Health Connect (which replaced Google Fit APIs), continuous glucose monitors, smart rings, blood pressure cuffs, your platform needs to ingest, normalize, and surface data from multiple sources. We’ve developed a reusable approach to wearable and device integrations because multiple longevity and clinical clients need the same capability: accelerated device onboarding and data normalization.
Three patterns derail most wearable integration efforts.
First, teams align wearable data with their existing clinical data structures. Those structures are built for episodic encounters, not continuous sensor streams. Longitudinal wearable data needs its own ingestion, storage, and retrieval patterns.
Second, teams underestimate the volume and noise of sensor data and the engineering effort required to make it clinically actionable. Raw accelerometer or PPG readings need significant processing before they mean anything to a patient or a clinician.
Third, teams assume rich third-party sensor data will keep flowing freely. It won’t. Apple, Google, and major device manufacturers control API access, data granularity, and pricing. Build a contingency for every data source you don’t control.
EHR Integration (Not Optional)
Whether it’s Epic, Athena, or Cerner, your longevity platform needs to read from and write to the clinical record. This isn’t a nice-to-have for Phase 2. It’s a Day 1 architectural decision. We’ve repeatedly focused on mitigating integration-related technical debt before scaling, because that debt compounds faster than any other kind.
Personalization Engine
Personalization isn’t a feature set. It’s a compliant strategy, design, and data structure for gathering the user-specific signal that drives both current engagement and future features. Health-related recommendations, risk flags, and clinical alerts are the obvious surface. Less obvious: analytics that tell you which next personalization strategy will best engage and retain users, so you can collect the right data in a compliant way and ship the next feature faster. One health plan app we built uses psychographic segmentation to place members into one of five behavioral segments, each receiving tone-matched and frequency-matched notifications. It’s a less common form of personalization in this space, and one Sidebench has unique experience with. The result: higher adherence rates and meaningful engagement with preventive care plans over 12-week cycles.
Research-Grade Data Export
Health systems launching longevity arms want the data they’re collecting to feed research programs. That means e-consent integration, offline-ready survey tooling, wearable normalization, and exportable data pipelines. We’ve built these capabilities for a health system research institute running individualized longevity studies, personalized research at scale.
AI with Human-in-the-Loop QA
If your longevity platform uses AI for recommendations, risk scoring, or clinical decision support, you need explicit human review workflows. UX flows and admin dashboards that surface AI confidence scores, allow clinician override, and log audit trails for clinical liability mitigation. This isn’t a compliance checkbox. It’s the trust architecture that determines whether clinicians actually use your platform.
Case Study Evidence: De-Risked Longevity Projects
The difference between longevity technology projects that succeed and those that don’t comes down to one thing: whether the team invested in strategy, architecture, and validation before development. Here’s what that looks like across four different segments, drawn from projects we’ve delivered.
| Client | Segment | Delivered by Strategic Partner (Sidebench) | Key Outcome |
|---|---|---|---|
| A major regional hospital system | Health System Preventive Care | Product and technical assessment, Epic integration risk audit, prioritized roadmap, RACI | Web platform architecture validated 10x-25x patient scale. Surfaced 3 critical architecture gaps that would have blocked scaling. |
| A cardiocognitive longevity clinic | Concierge / Clinical | Product discovery, AthenaOne strategy, device inventory, user research, validated with real ICP user testing | From concept to implementation-ready architecture in 6 weeks. Validated with target patients before a single line of code. |
| A consumer longevity membership brand | Direct-to-Consumer | Mobile-first platform redesign, brand integration, AI triage integration, conversion optimization, growth plan | Growth plan targeting 12,000+ members. Doubled membership through UX and conversion work. |
| A health system research institute | Individualized Medicine / Research | End-to-end product specification and technical architecture for a precision medicine research platform, with wearable data ingestion, lab uploads, and researcher-facing tooling | Platform for personalized longevity studies at scale. Clinical rigor meets research velocity. |
The Build vs. Partner Decision
You’re going to build longevity technology. The question is whether you build it with an internal team, an offshore shop, or a strategic product partner. Each path carries different risk, cost, and speed tradeoffs, and the right choice depends on how much product strategy work you’ve already done.
The framing depends on which stage you’re in. Initial product vision should always come from your internal team, no partner should be shaping that for you. The first real gate is whether to invest in a full strategy and design phase at all, or go straight to implementation. If you commit to strategy and design, the second gate is whether to run it internally, with an experienced strategic partner, or with a dev shop. A dev shop will usually build whatever you think you want, without challenging the UX, strategy, data model, or integration assumptions. A strategic partner is worth the premium precisely when those assumptions need pressure-testing.
| Internal Team | Offshore Dev Shop | Strategic Product Partner | |
|---|---|---|---|
| Product strategy | You own it entirely | You provide it, they execute | Co-created with you |
| Compliance risk | Depends on team experience | High (distance from US regs) | Low (embedded in process) |
| Speed to prototype | Slow (hiring + ramp) | Fast (but quality risk) | Fast (experienced teams) |
| EHR integration | If you have the expertise | Rare capability offshore | Core competency for top firms |
| Cost | Highest (salaries + benefits) | Lowest hourly, often highest total | Premium but predictable |
| De-risking | You bear all risk | They bear none | Shared accountability |
One additional option: hybrid models that pair US-based health tech strategy and technical architecture leads with managed offshore engineering teams can mitigate compliance and integration risks while staying more cost-effective. The key is that the onshore team retains full technical authority over architecture decisions, compliance review, and client-facing communication. The cost advantage is real; the risk only materializes when offshore teams operate without that structural oversight.
The firms that position themselves as “app developers” will give you exactly what you asked for, even if what you asked for is wrong. A strategic product partner challenges your assumptions, surfaces risks you haven’t considered, and helps you build the right product before building the product right.
Planning a Longevity Technology Investment?
We’ve de-risked longevity technology projects for health systems, concierge clinics, and consumer platforms. If you’re building the business case, we can help you pressure-test the framework before you commit to the build.
Get a longevity-program readiness assessment from the team behind Hoag Compass →
FAQ
What’s the minimum viable investment for a longevity technology platform?
A discovery and de-risking phase typically runs $50K-$150K over 4-8 weeks. MVP development adds $200K-$500K over 12-20 weeks. Total minimum viable investment: $250K-$650K to get a working product with validated demand.
How long does EHR integration take for longevity platforms?
Plan for 3-6 months for Epic integration, 2-4 months for Athena. These timelines assume you’ve done the architecture work upfront. Without discovery, double them.
Do we need HIPAA compliance for a consumer longevity app?
If you’re handling any health data, wearable readings, lab results, health assessments, yes. HIPAA applies the moment you’re a covered entity or business associate handling protected health information (PHI). Don’t build a longevity platform and assume you can add compliance later.
Should we build our own wearable integration layer or use a third-party service?
It depends on how central wearable data is to your product. If it’s your core value proposition, owning the integration layer gives you control and differentiation. If it’s supplementary, a third-party service gets you there faster.
What’s the biggest risk in longevity technology projects?
Building before validating. Teams that skip the Discovery, Strategy, and Validation phase and jump straight to development consistently spend 3-5x more than teams that invest 6-8 weeks in product validation, technical architecture, and prototype testing.
How do we measure ROI on a longevity technology investment?
Track three tiers: (1) engagement metrics, active users, session frequency, device data submissions; (2) clinical outcomes, adherence rates, risk score improvements, preventive care utilization; (3) business outcomes, patient retention, new patient acquisition, revenue per member, payer contract value.
Can we start with a limited pilot and expand later?
Yes, and you should. But “limited pilot” doesn’t mean “quick and dirty.” The architecture decisions you make for 500 users need to support 50,000. Discovery surfaces these architectural constraints before they become technical debt.
What makes longevity technology different from standard healthcare apps?
Three things: (1) longitudinal data requirements, you’re tracking patients over years, not episodes; (2) multi-source data integration, wearables, labs, genomics, lifestyle; (3) consumer-grade UX expectations, longevity patients are health-motivated and comparing your platform to consumer wellness apps. Clinical accuracy with consumer polish is the bar.
How do we handle AI features in a HIPAA-compliant longevity platform?
Build explicit human-in-the-loop workflows. AI generates recommendations, humans review them, and audit trails log every decision. Design admin dashboards that surface AI confidence scores and allow clinician override. Don’t ship AI features without a documented QA workflow.
What should we look for in a longevity technology partner?
Five things: (1) experience building in regulated health tech, not just general software; (2) a discovery-first approach that validates before building; (3) EHR integration as a core capability, not a subcontracted feature; (4) quantified outcomes from previous projects, not just portfolio screenshots; (5) willingness to challenge your assumptions and tell you when your product concept needs rethinking.
Cited Data Sources
- Grand View Research, 2024, Global longevity and anti-aging market projections
- Google Developer Documentation, 2024, Google Fit deprecation timeline
- HHS.gov, HIPAA Security Rule (45 CFR 164.312)
- IBM, 2024, Cost of a Data Breach Report
- FDA, 2025, AI/ML-Enabled Medical Devices
About the Author
Kevin Yamazaki is Partner and CEO at Sidebench, a Los Angeles-based digital transformation consultancy and product studio. Under his leadership, Sidebench has delivered 60+ healthcare implementations spanning HIPAA-compliant architecture, EHR integrations, and platforms handling millions of patient appointments annually. Sidebench has also made 14 health tech investments at Seed, A, B, and C stages alongside client engagements, including in Cortica and NOCD, aligning incentives with operators it builds with. Cross-industry partners include Oakley, Red Bull, and Cedars-Sinai. sidebench.com