The FDA has now cleared over 1,000 AI-enabled medical devices as of 2025, AI-driven drug discovery is compressing development timelines from 10+ years to under 5, and health systems are deploying ambient clinical documentation that saves physicians 2+ hours of charting daily. The global healthcare AI market is projected to reach $45.2 billion by 2026 (Statista). This article cuts through the hype to explain what’s actually working, what’s coming next, and what technology leaders need to know.
Healthcare Implementations
Platform Users Scaled
Compliant Architecture
Client Value Created
Last updated: February 2026
By: Kevin Yamazaki, Partner, CEO at Sidebench
In this article:
- Healthcare AI News: Key Developments in 2026
- What Are the Biggest AI Healthcare Trends in 2026?
- How Does AI Reduce Healthcare Administrative Costs?
- How Is AI Transforming Emergency Medicine?
- How Is AI Accelerating Drug Discovery?
- How Is AI Improving Cancer Detection and Treatment?
- How Does AI Reduce Medical Errors in Diagnostics?
- How Does AI Predict Patient Risk and Prevent Readmissions?
- What AI-Powered Medical Devices Are Changing Healthcare?
- What Does the Future of AI in Healthcare Look Like?
- Comparison Tables
- FAQ
Healthcare AI News: Key Developments in 2026
Healthcare AI in 2026 is defined by three major shifts: ambient documentation going mainstream, diagnostic AI moving from radiology into new specialties, and the FDA’s evolving approach to continuous learning systems.
Ambient Clinical Documentation Adoption Accelerates
Ambient AI scribes — systems that listen to patient-physician conversations and automatically generate clinical notes — have moved from pilot to production. Nuance DAX, Abridge, and Suki are now deployed across thousands of physicians, with reported time savings of 2+ hours daily per clinician. The economics are compelling: at $50K-$150K annually, these systems pay for themselves if they prevent even one physician from burning out.
Diagnostic AI Expands Beyond Radiology
While radiology remains the most mature application, 2026 is seeing diagnostic AI move into pathology, ophthalmology, and dermatology. The Swedish MASAI trial published in Lancet Digital Health found that AI-supported mammography screening detected more cancers while maintaining comparable specificity to standard double reading. But integration with existing PACS and EHR systems determines success more than algorithm performance.
FDA Clarity on Continuous Learning
The FDA issued updated guidance on AI systems that continue learning after deployment. The emerging answer: if the update changes the intended use or significantly alters performance, it triggers review. If it’s routine maintenance, it may not. This clarity is enabling vendors to plan continuous improvement pathways.
What Are the Biggest AI Healthcare Trends in 2026?
AI in healthcare is consolidating around six major application areas, each at different maturity levels. The trend is clear: AI is moving from “interesting pilot” to “operational necessity” in documentation and diagnostics.
| Application | Maturity | Impact | Typical Cost |
|---|---|---|---|
| Ambient documentation | Production | 2+ hrs/day saved | $50K-$150K/yr |
| Diagnostic imaging | Production | 5-15% accuracy gain | $100K-$500K |
| Drug discovery | Growth | 30-50% timeline cut | $1M+ |
| Predictive analytics | Production | 20-30% fewer adverse events | $100K-$500K |
| Admin automation | Growth | 15-30% cost reduction | $50K-$300K |
| Robotic surgery | Early | Improved precision | $1M+ |
How Does AI Reduce Healthcare Administrative Costs?
Healthcare administrative costs consume 15-30% of total spending — over $1 trillion annually in the US (JAMA, Sahni et al., 2019). AI targets several high-cost activities where manual processes create bottlenecks and errors.
Clinical Documentation
Before ambient AI, physicians spent 2+ hours daily on clinical documentation — time that contributed to burnout. Ambient systems reduce this to review-and-sign, fundamentally changing the physician workday.
Coding and Billing
Manual coding error rates typically range from 7% to 25% depending on coder expertise and documentation quality (AHIMA). AI vendors report substantially lower error rates, though independent peer-reviewed validation is still emerging.
Prior Authorisation
Some payers now accept AI-generated prior authorisation requests, with near-instant approval for cases meeting criteria. Prior auth consumes an average of 13 hours per physician per week (AMA 2024 Prior Authorization Physician Survey), eating into time that should go toward patient care.
Scheduling Optimisation
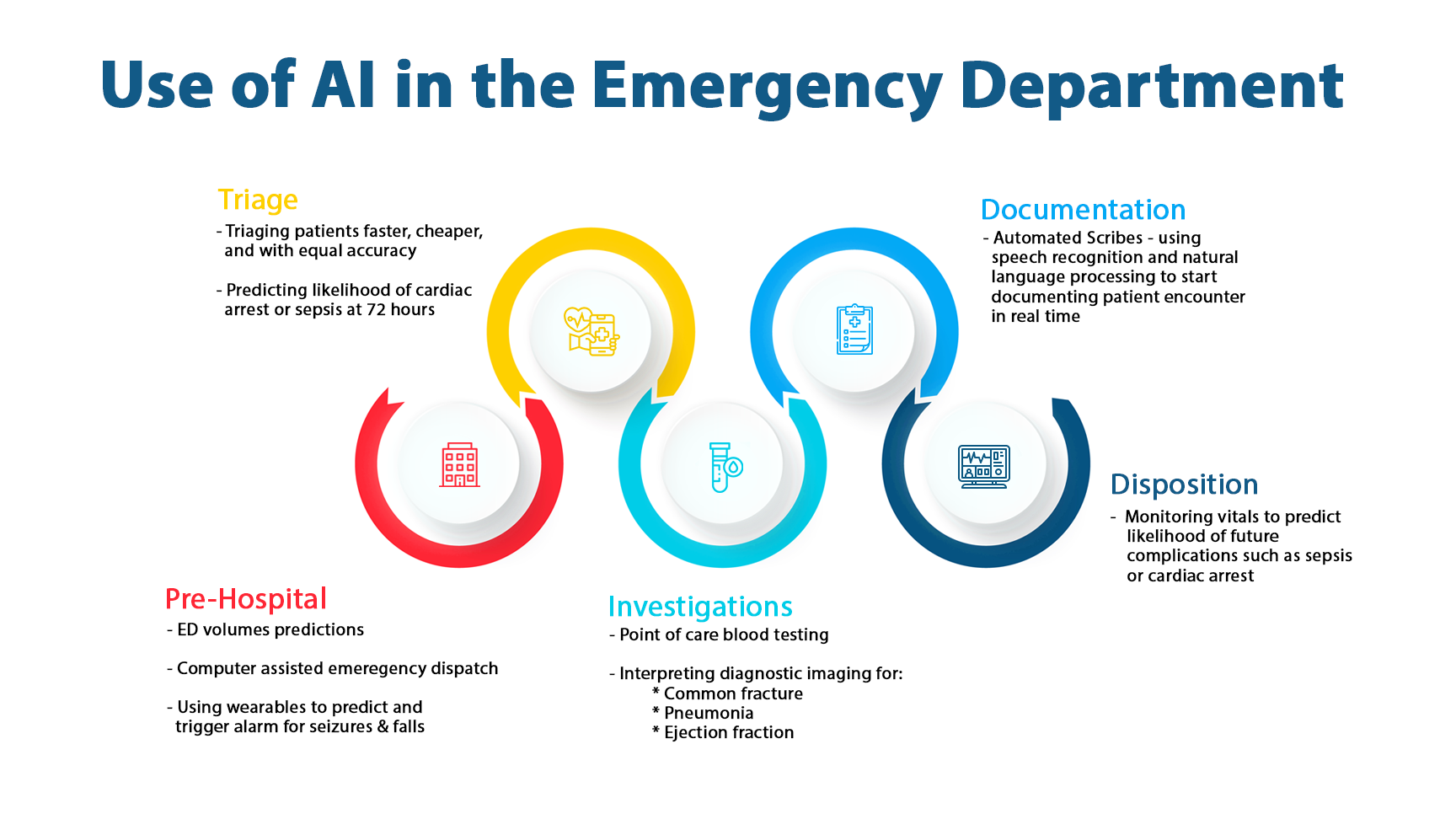
How Is AI Transforming Emergency Medicine?
Emergency departments face a fundamental challenge: triaging patients accurately when information is incomplete and time is critical. AI addresses this through predictive triage, sepsis detection, and imaging prioritisation.
Predictive Triage
AI analyses vital signs, chief complaint, and available history to predict deterioration risk. High-risk patients are flagged for immediate attention, even if their current presentation seems stable.
Sepsis Early Warning
Sepsis contributes to at least 350,000 deaths among American adults annually (CDC), and early intervention dramatically improves outcomes. AI systems monitoring real-time vital signs can detect sepsis 4-6 hours before clinical recognition, enabling earlier antibiotic administration.
Imaging Prioritisation
AI pre-screens imaging studies, flagging critical findings (stroke, PE, pneumothorax) so radiologists review the most urgent cases first. In stroke, where “time is brain,” this can shave minutes off treatment delays.
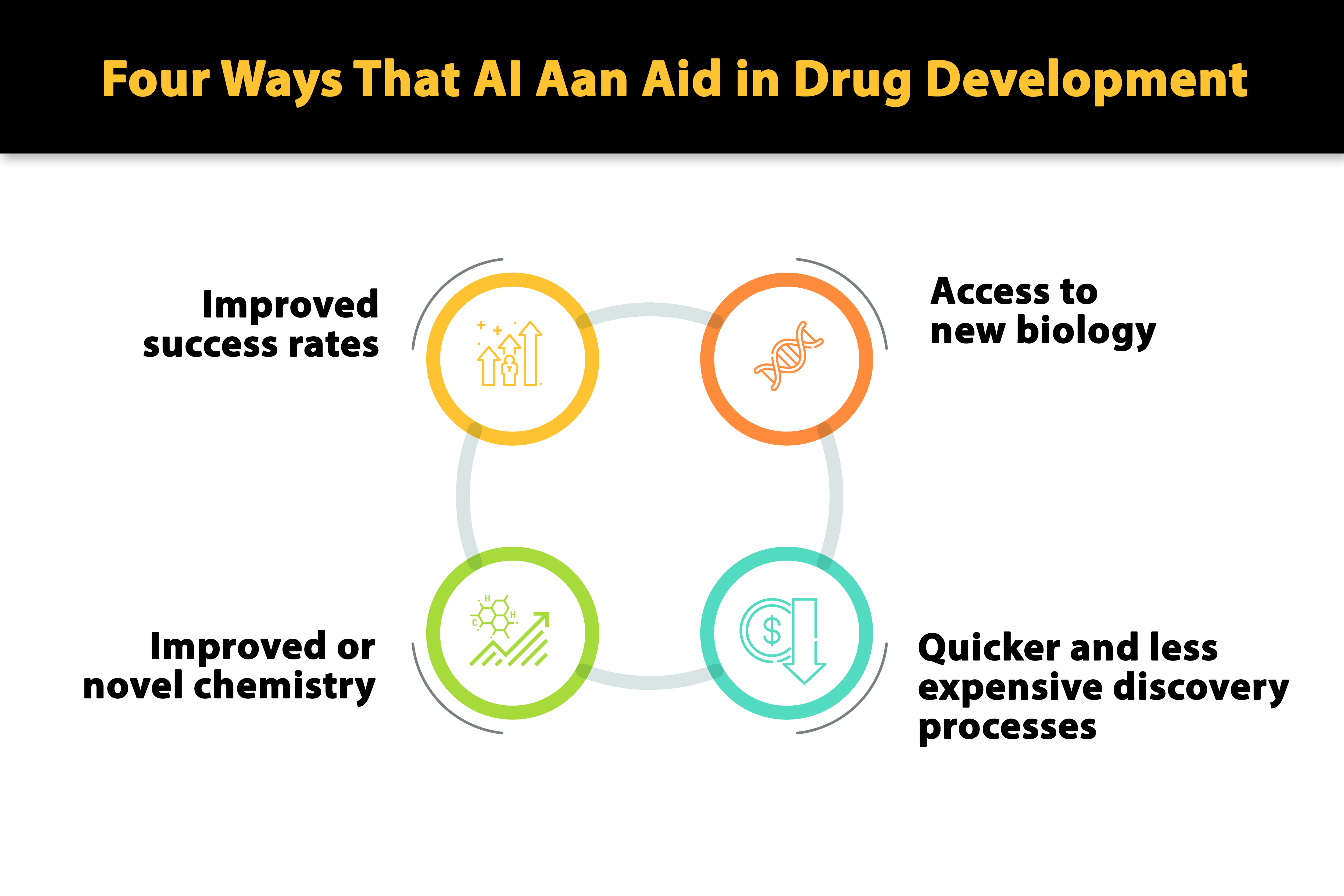 How Is AI Accelerating Drug Discovery?
How Is AI Accelerating Drug Discovery?
Traditional drug development takes 10-15 years and costs $2.6 billion per approved drug (Tufts CSDD, DiMasi et al., 2016). AI is compressing this timeline through molecular modelling, clinical trial optimisation, and drug repurposing.
Molecular Modelling
AI analyses molecular structures and predicts drug-target interactions, identifying promising candidates faster than traditional screening. What once took months of lab work can now be simulated in hours.
Clinical Trial Optimisation
AI identifies eligible patients for clinical trials, predicts likely responders, and optimises trial design to reach statistical significance with smaller populations.
Drug Repurposing
AI analyses existing approved drugs to identify new therapeutic applications. This is faster and cheaper than developing new molecules — the safety profile is already established.
 How Is AI Improving Cancer Detection and Treatment?
How Is AI Improving Cancer Detection and Treatment?
Cancer diagnosis relies on pattern recognition — exactly where AI excels. AI-supported screening, pathology analysis, and treatment response prediction are reshaping oncology workflows.
Mammography Screening
The MASAI trial published in Lancet Digital Health demonstrated that AI-supported mammography screening detected more invasive cancers compared to standard double reading, while using 44% fewer screen readings. Radiologists using AI as a “second reader” outperform either alone.
Pathology Analysis
AI analyses tissue samples for cancer markers, detecting patterns invisible to human observers. This is particularly valuable in prostate cancer grading, where inter-observer variability among pathologists is high.
Treatment Response Prediction
AI predicts which patients will respond to specific treatments based on tumour genetics, previous treatment history, and population-level outcomes data.
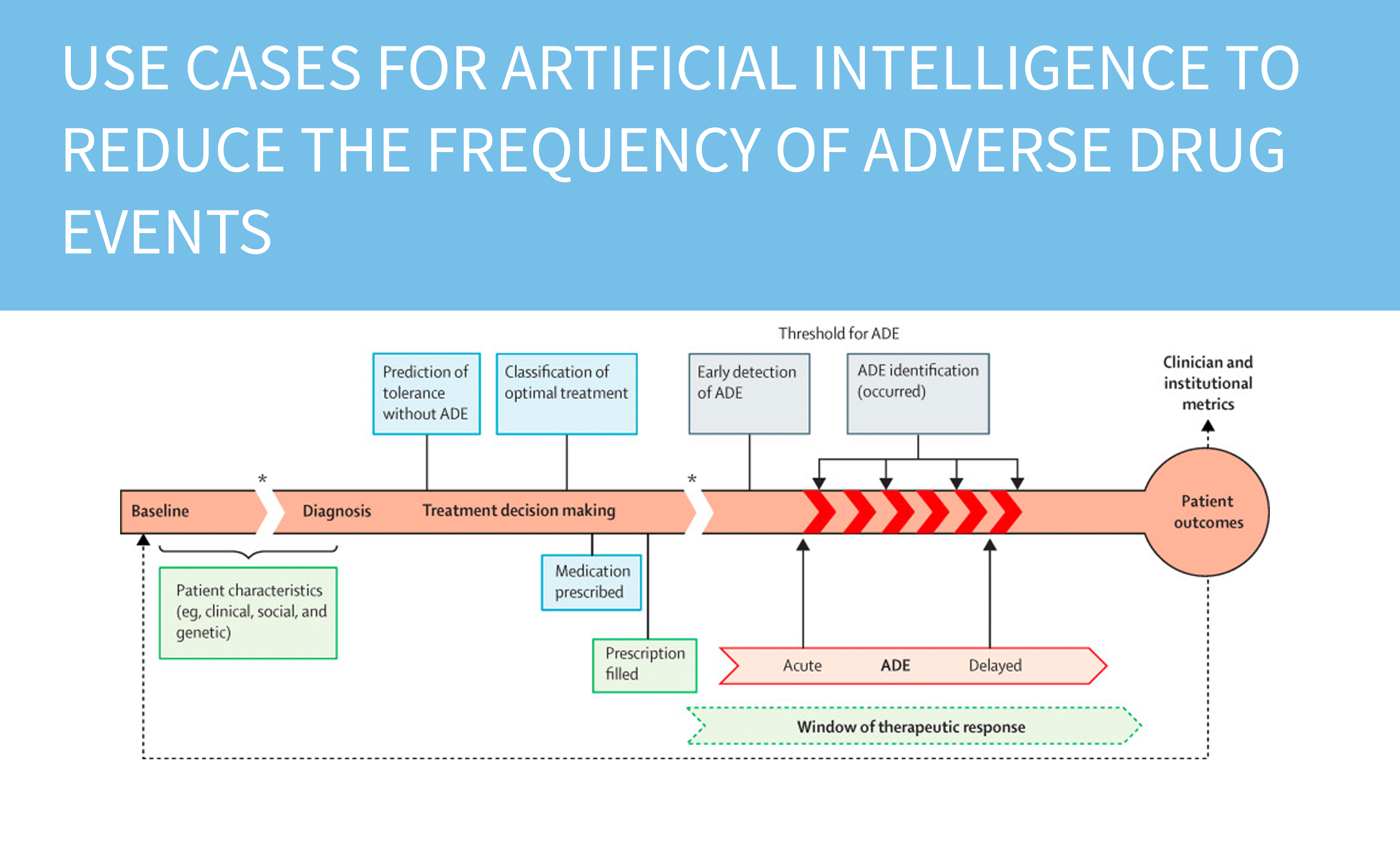 How Does AI Reduce Medical Errors in Diagnostics?
How Does AI Reduce Medical Errors in Diagnostics?
Medical errors cause an estimated 250,000 deaths among Americans annually — the third leading cause of death (BMJ, Makary & Daniel, 2016). AI addresses this through medication checking, diagnostic decision support, and radiology quality assurance.
Medication Interaction Checking
AI-powered systems check every prescription against the patient’s full medication list, flagging dangerous interactions before the order is signed. Clinical decision support systems have been shown to reduce medication errors, though precise numbers vary by implementation.
Diagnostic Decision Support
AI analyses patient symptoms, lab values, and imaging against databases of millions of cases, suggesting diagnoses that clinicians might miss. This is particularly valuable for rare conditions where individual physician experience is limited.
Radiology Quality Assurance
AI reviews radiology interpretations, flagging potential misses for second review. This catches errors before they reach patients.
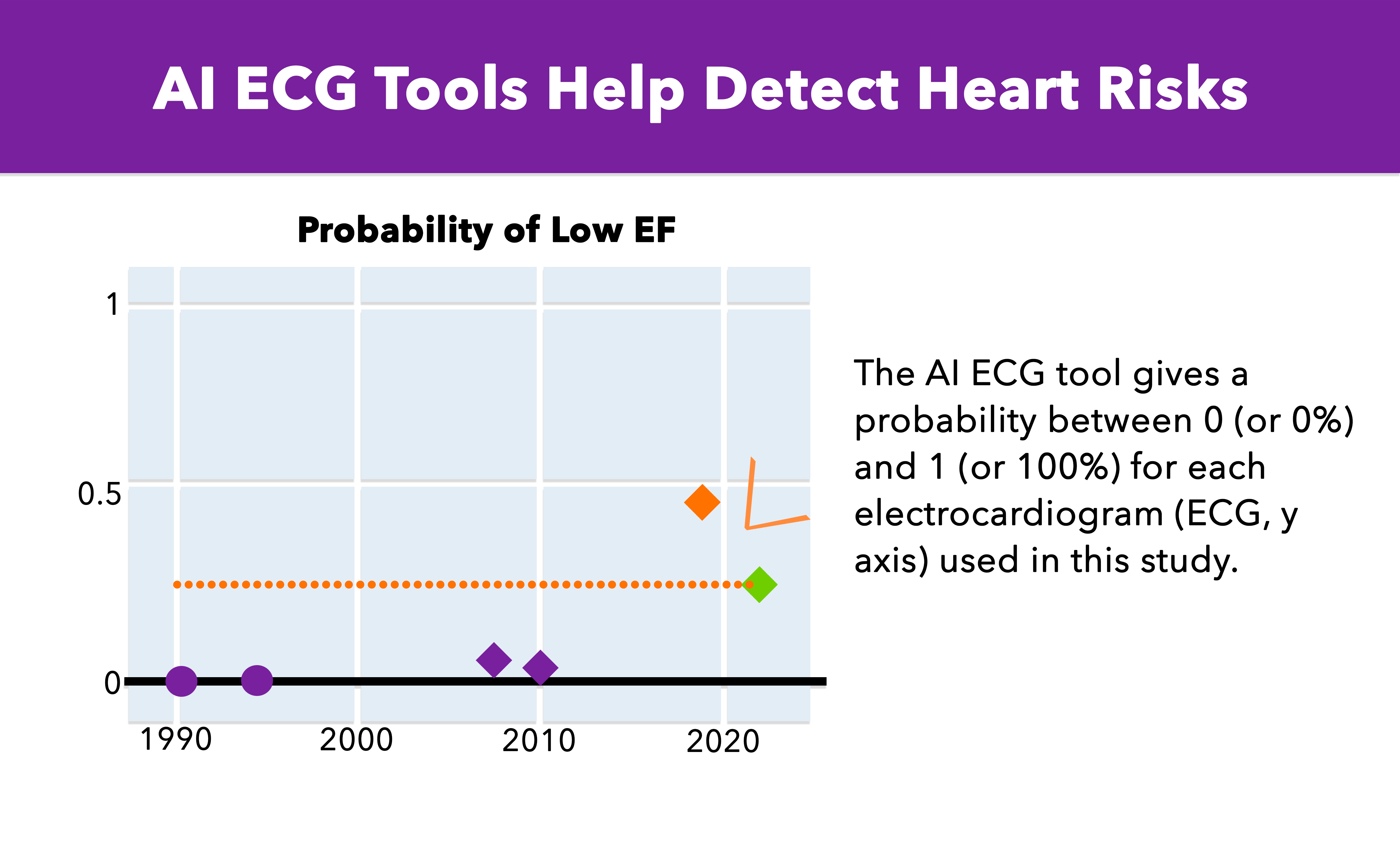 How Does AI Predict Patient Risk and Prevent Readmissions?
How Does AI Predict Patient Risk and Prevent Readmissions?
Hospital readmissions cost Medicare $26 billion annually (CMS/MedPAC), and a significant portion are preventable. AI targets readmission risk through predictive modelling, remote monitoring, and care gap identification.
Risk Stratification
AI identifies high-risk patients before discharge, enabling targeted interventions: additional education, home health referrals, earlier follow-up appointments.
Remote Monitoring
AI analyses data from home monitoring devices (blood pressure, weight, glucose), detecting concerning trends before they become emergencies.
Care Gap Identification
AI identifies patients overdue for preventive care — screenings, immunisations, chronic disease management — enabling proactive outreach.
What AI-Powered Medical Devices Are Changing Healthcare?
The FDA has cleared over 1,000 AI-enabled medical devices across multiple categories as of 2025. Most fall into diagnostic aids and clinical decision support.
| Category | Examples | FDA Cleared |
|---|---|---|
| Radiology | IDx-DR, Viz.ai, Zebra | 500+ |
| Cardiology | Eko, AliveCor, Caption | 100+ |
| Pathology | Paige, PathAI | 30+ |
| Ophthalmology | IDx-DR, EyeArt | 20+ |
| Dermatology | DermaSensor, SkinVision | 10+ |
What Does the Future of AI in Healthcare Look Like?
Healthcare AI is evolving along several trajectories, with near-term adoption in documentation and diagnostics while longer-term challenges around bias and liability remain.
Near-Term (2026-2028)
- Ambient documentation becomes standard of care
- AI diagnostic aids required for reimbursement in certain specialties
- Continuous learning systems with FDA-approved update pathways
Medium-Term (2028-2030)
- AI-first clinical workflows (AI generates, human reviews)
- Personalised treatment protocols based on individual patient data
- AI-managed chronic disease programs with autonomous escalation
Long-Term Challenges
- Algorithmic bias from unrepresentative training data
- Liability uncertainty when AI contributes to clinical errors
- Workforce transition as AI automates administrative tasks
- Data privacy in an era of large-scale AI training
Comparison Tables
AI Applications by Healthcare Function
| Function | AI Application | Maturity | Impact |
|---|---|---|---|
| Diagnostics | Image analysis, pathology | Production | 5-15% accuracy gain |
| Drug Discovery | Molecular modelling | Growth | 30-50% timeline cut |
| Documentation | Ambient AI scribes | Production | 2+ hrs/day saved |
| Predictive | Readmission, sepsis | Production | 20-30% fewer events |
| Administrative | Coding, billing, scheduling | Growth | 15-30% cost cut |
| Surgery | Robotic assistance | Early | Improved precision |
Current vs. AI-Enhanced Healthcare Workflows
| Workflow | Without AI | With AI |
|---|---|---|
| Radiology reading | 15-20 min per study | 3-5 min with AI pre-screen |
| Clinical documentation | 2+ hours/day manual | Real-time ambient |
| Drug interaction check | Manual pharmacy review | Automated real-time alerts |
| Patient triage | Nurse assessment, wait | AI risk scoring, priority routing |
| Billing & coding | Manual, 7-25% error rate | AI-assisted, improved accuracy |
FAQ
What is AI in healthcare?
AI in healthcare uses machine learning, natural language processing, and computer vision to analyse medical data, support clinical decisions, and automate administrative tasks. Applications range from diagnostic imaging analysis to drug discovery, predictive analytics, and virtual health assistants.
How is AI used in hospitals today?
Hospitals use AI for diagnostic imaging (detecting tumours and fractures), clinical documentation (ambient AI scribes), bed management, sepsis prediction, medication interaction checking, pathology analysis, and administrative automation including coding, billing, and scheduling.
Will AI replace doctors?
AI is unlikely to replace physicians but will augment their capabilities. AI excels at pattern recognition in large datasets but lacks clinical judgement and empathy. The most effective model is AI-assisted clinical decision-making where technology handles data processing and clinicians make final decisions.
What are the risks of AI in healthcare?
Key risks include algorithmic bias from unrepresentative training data, liability uncertainty when AI contributes to clinical errors, data privacy concerns, over-reliance on AI recommendations, regulatory gaps in oversight, and potential for AI systems to perpetuate existing health disparities.
How does AI improve drug discovery?
AI analyses molecular structures, predicts drug-target interactions, and simulates clinical outcomes to identify candidates faster. Traditional development takes 10-15 years; AI reduces this by 30-50%. AI also identifies existing approved drugs effective for new indications (drug repurposing).
Is AI in healthcare regulated?
Yes. The FDA regulates AI-enabled medical devices through 510(k), De Novo, and PMA pathways. Over 1,000 devices have clearance as of 2025. The EU AI Act classifies healthcare AI as “high-risk.” HIPAA applies to AI systems processing protected health information.
What is ambient clinical documentation?
Ambient clinical documentation uses AI to listen to patient-physician conversations and automatically generate clinical notes, saving physicians 2+ hours daily. Systems like Nuance DAX, Abridge, and Suki process natural speech and structure it into EHR-compatible medical records.
How accurate is AI in medical imaging?
AI diagnostic accuracy varies by application but increasingly matches human performance. The MASAI trial found AI-supported screening detected more cancers than standard double reading. AI performs best as a “second reader” alongside radiologists rather than as a replacement.
What is predictive analytics in healthcare?
Predictive analytics uses machine learning to forecast patient outcomes from historical data. Applications include predicting readmission risk, identifying sepsis early, forecasting disease progression, optimising staffing levels, and anticipating supply chain needs.
How much does AI cost to implement in healthcare?
Costs vary widely: ambient documentation ($50-150K/year), diagnostic AI ($100K-500K per system), custom AI platforms ($200K-2M+). ROI typically materialises through reduced administrative costs, fewer errors, and improved throughput.
Sidebench Perspective
AI implementation in healthcare fails when organisations focus on the technology instead of the workflow. We’ve seen million-dollar AI investments sit unused because they added steps to clinician workflows rather than removing them. Deploying clinical AI also requires HIPAA-compliant implementation from day one — not bolted on afterward. Start with the workflow problem — documentation burden, diagnostic uncertainty, scheduling complexity — and then evaluate whether AI is the right solution. AI is already making a real difference in scaling behavioral health technology through scheduling optimisation and intake automation. Sometimes AI is the answer. Sometimes a simpler approach works better.
Planning an AI Implementation?
Sidebench has delivered AI-assisted platforms for behavioral health, health plans, and provider groups. Start with our healthcare technology partner evaluation framework or talk to us directly.
Cited Data Sources
- FDA AI/ML-Enabled Medical Devices — FDA: AI/ML-Enabled Medical Devices
- Healthcare AI Market Size (Statista) — Statista: Healthcare AI Market Forecast
- Healthcare Administrative Costs (JAMA 2019) — Sahni NR, et al. “Administrative Simplification and the Potential for Saving a Quarter-Trillion Dollars in Health Care.” JAMA, 2019.
- AMA Prior Authorization Survey 2024 — AMA: 2024 Prior Authorization Physician Survey
- CDC Sepsis Data — CDC: Sepsis — About
- Drug Development Costs (Tufts CSDD) — DiMasi JA, et al. “Innovation in the pharmaceutical industry.” Journal of Health Economics, 2016.
- Medical Errors (BMJ 2016) — Makary MA, Daniel M. “Medical error — the third leading cause of death in the US.” BMJ, 2016;353:i2139.
- Hospital Readmissions (CMS/MedPAC) — MedPAC: Hospital Readmissions Reduction Program
- MASAI Trial (Lancet Digital Health) — Lang K, et al. “AI-supported screen reading versus standard double reading in the MASAI trial.” Lancet Digital Health, 2023.
- FDA PCCP Guidance — FDA: Marketing Submission Recommendations for PCCP
About the Author
Kevin Yamazaki is Partner and CEO at Sidebench, a Los Angeles-based digital transformation consultancy and product studio. He has led healthcare technology implementations for organisations including Children’s Hospital Los Angeles, IEHP, Hoag, and Cortica, spanning HIPAA-compliant architecture, EHR integrations, and healthcare platform development. Under his leadership, Sidebench has delivered 50+ healthcare implementations, including platforms handling over 1 million patient appointments annually.